Bloating after meals. Skin flare-ups that don’t track neatly with any one food. Fatigue that feels disproportionate to how you’re eating. You’ve probably already tried the obvious steps, including basic diet changes, supplements, and standard testing, only to end up with partial answers.
That’s why so many people searching for microbiome testing australia aren’t looking for another wellness trend. They want a test that explains something useful. They want to know whether the problem is microbial imbalance, infection, food-related immune activation, impaired tolerance to histamine, or a mix of several factors.
The difficulty is that “microbiome testing” now covers very different technologies, very different clinical standards, and very different levels of interpretation. Some tests are broad but shallow. Some are narrow but clinically helpful. Some are sold as lifestyle products when they really need practitioner interpretation to be useful.
An Introduction to Microbiome Testing in Australia
Australia’s interest in gut health isn’t niche. A 2024 analysis of Google Trends reported that Australia ranked first worldwide for searches related to microbiome and gut health. That level of public interest reflects something clinicians see every day. People are trying to connect chronic symptoms with something more specific than “sensitive stomach” or “inflammation”.
Microbiome testing can be useful, but only if you understand what question the test is answering. A stool test can show patterns in the gut ecosystem. It may identify low diversity, over-representation of opportunistic organisms, or markers that support further medical review. What it usually can’t do on its own is explain every trigger behind the pattern.
That distinction matters. Patients often arrive with a report that labels microbes as “good” or “bad” but doesn’t tell them what to change, what to ignore, or what needs proper medical follow-up. The report may be technically accurate and still clinically incomplete.
Why the current landscape feels confusing
The Australian market includes practitioner-led tests, direct-to-consumer options, targeted pathogen panels, and broader sequencing platforms. They don’t all serve the same purpose.
A useful way to think about the field is this:
- Some tests screen for known suspects: These are best when infection, parasites, viruses, or specific opportunistic organisms are the main concern.
- Some tests map the whole ecosystem: These are better when the question is broader, such as long-term dysbiosis, functional capacity, or patterns linked to chronic symptoms.
- Some tests are only one part of the picture: They can reveal what the gut looks like, but not always why it became imbalanced.
Clinical reality: A sophisticated report doesn’t automatically create a useful treatment plan. Interpretation quality matters as much as laboratory method.
If you’re trying to decide whether testing is worth it, the answer depends less on the brand and more on the diagnostic pathway around it. The most productive approach usually starts with the symptom pattern, then selects the test type that can change management.
Understanding Your Gut Microbiome and Its Impact on Health
The gut microbiome is best understood as an internal ecosystem. It includes bacteria, fungi, archaea, viruses, and other microbes that live in the digestive tract. In a balanced state, these organisms help regulate digestion, immune signalling, barrier integrity, and metabolic activity. In an imbalanced state, those functions can become less stable.
Clinicians often use two terms here. Eubiosis means a more balanced microbial environment. Dysbiosis means the ecosystem has shifted in a less favourable direction. That shift might involve reduced diversity, low levels of beneficial organisms, or overgrowth of opportunistic species.
What dysbiosis can look like in practice
Dysbiosis doesn’t create one universal symptom pattern. In practice, people may report bloating, irregular bowel habits, abdominal discomfort, food reactivity, fatigue, or skin symptoms. The reason it becomes confusing is that the same symptom can arise from several pathways.
For example, bloating can occur with altered fermentation patterns, low digestive capacity, a reaction to specific foods, or a targeted pathogen issue. A microbiome test can help narrow the field, but it doesn’t replace clinical reasoning.
For readers wanting a broader foundation in daily gut-supportive habits, a comprehensive guide to good gut health gives a practical lifestyle overview that pairs well with formal testing. If you want a concise explanation of what these reports can reveal, this overview of what your gut microbiome reveals about your health is also useful context.
Why this matters medically, not just as a wellness topic
The microbiome matters because gut disorders aren’t trivial. In Australia, inflammatory bowel disease affects approximately 1 in 250 people, and the Australia IBD Microbiome Study has been developed to investigate microbiome links in these chronic diseases.
That doesn’t mean every person with bloating has IBD. It does mean microbiome science sits inside mainstream clinical relevance, not just wellness marketing.
A gut report is most useful when it helps separate ordinary fluctuation from a pattern that deserves proper investigation.
The main point patients often miss
A healthy microbiome isn’t about eliminating all microbes that sound unfamiliar. It’s about balance, resilience, and function. Some organisms are helpful in one context and problematic in another. Some findings matter only when they appear alongside symptoms, inflammation markers, or a consistent clinical history.
That’s why interpretation should move beyond “fix every red flag on the page”. The central question is whether the result explains your symptoms well enough to justify a targeted change.
The Different Types of Microbiome Tests Explained
Not all microbiome tests are doing the same job. This difference is a common source of confusion. Two stool tests can look similar on a website and be very different in what they measure, what they miss, and how useful they are in clinic.
A simple comparison helps.
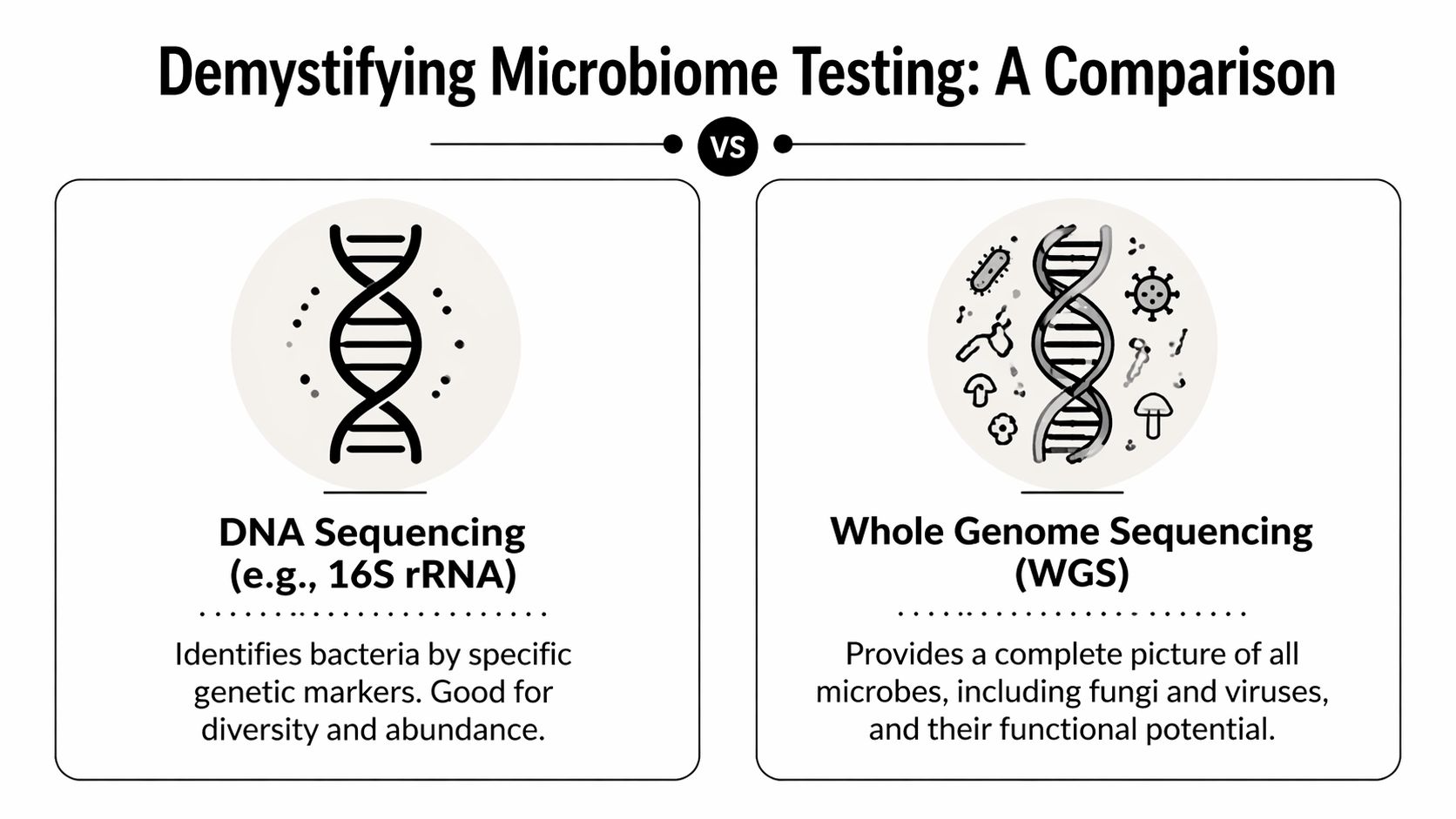
- 16S-style sequencing is like a census. It tells you which bacterial groups appear to be present.
- Targeted PCR panels are like a most-wanted list. They look hard for specific organisms already on the lab’s panel.
- Shotgun metagenomic sequencing is the most complete blueprint. It looks across all DNA in the sample and gives a broader map of both organisms and potential function.
16S testing and where it fits
16S sequencing is commonly used to identify bacterial patterns by analysing selected genetic markers. It can be helpful for broad ecological questions, especially when the goal is to look at overall diversity and relative abundance.
Its limitation is built into the method. It doesn’t give the same depth as whole-genome approaches, and it won’t give a full view of non-bacterial organisms or functional genes in the same way. For some patients, that’s acceptable. For others, it leaves too many unanswered questions.
This type of test is often enough when the clinician wants a high-level view rather than a highly actionable pathogen or function-focused analysis.
Targeted PCR panels and when they work well
PCR-based tests are narrow by design, and that’s not a weakness when the question is specific. If a patient has symptoms that suggest infection, parasite burden, fungal overgrowth, or a targeted opportunistic issue, PCR can be very useful.
The advantage is sensitivity for the organisms on the panel. According to Australian testing content on this category, the Complete Microbiome Mapping approach uses PCR-based DNA detection from a stool sample to screen for pathogenic bacteria, commensal bacteria, opportunistic pathogens, fungi, viruses, parasites, and immune or digestive markers, with a reported turnaround of 7 to 10 days through the provider described on that page. The same source notes that this format is designed for broad pathogen screening and low-level detection within its defined panel, via the Australian overview of Complete Microbiome Mapping.
What PCR won’t do is tell you much about organisms that aren’t on the panel. If the question is “what’s the broader architecture of this gut ecosystem?”, PCR is not the best fit.
Shotgun metagenomics and why it gets attention
Shotgun metagenomic sequencing is currently the most information-rich option in the consumer and practitioner market. Australian providers describe it as sequencing all DNA in the stool sample, rather than selected targets. In the source material available for this article, this method is described as capable of profiling over 28,000 microbial species, including bacteria, archaea, fungi, parasites, and protists, while also examining functional genes. That description appears in this Australian overview of shotgun metagenomic microbiome testing.
That functional layer matters. It shifts the result from “who is there” to something closer to “what this ecosystem may be capable of doing”.
Practical rule: Use shotgun metagenomics when the question is broad, persistent, and pattern-based. Use targeted PCR when you need to rule in or rule out defined organisms.
A side-by-side comparison
| Test type | Best use | Strength | Main limitation |
|---|---|---|---|
| 16S-style sequencing | Broad diversity view | Useful ecological overview | Less complete and less function-rich |
| Targeted PCR | Known pathogens or specific suspects | Sensitive within a defined panel | Misses organisms outside that panel |
| Shotgun metagenomics | Complex chronic symptom patterns | Broad species detection and functional insight | Usually needs better interpretation to be useful |
What usually doesn’t work
What doesn’t work is choosing a test because the report looks impressive. A patient with suspected parasite exposure, post-infectious symptoms, or a strong pathogen question may get more value from a high-quality targeted PCR panel than from a broad sequencing report. A patient with long-standing digestive instability, food reactivity, and non-specific systemic symptoms may need the opposite.
The best test is not the most marketed one. It’s the one that changes the next clinical decision.
How to Choose a Reputable Australian Testing Provider
Once you know the difference between methods, the next decision is provider quality. This matters more than many people realise. A technically strong method can still produce an unhelpful clinical experience if the collection pathway, sample handling, or interpretation process is weak.
One basic divide in Australia is direct-to-consumer convenience versus practitioner-led testing. Both exist. According to Australian microbiome testing commentary, some tests are available without referral, while many others require a qualified practitioner and are used inside a broader clinical plan, as discussed in this overview of microbiome PCR testing pathways in Australia.
What to check before ordering
If you’re comparing providers, start with these criteria:
- Laboratory standards: Look for accredited or clearly quality-managed processing. If a provider is vague about laboratory handling, that’s a concern.
- Method transparency: The provider should state whether the test is PCR, 16S-style sequencing, or shotgun metagenomics.
- Clinical interpretation: Ask who explains the report and whether that person can integrate symptoms, medical history, and follow-up action.
- Sample logistics: Stable collection and transport matter. This is one reason pathology collection and clinical-grade handling remain important in adjacent testing categories.
- Actionability: A useful report should lead to a structured next step, not a long list of supplements with no rationale.
Why practitioner involvement often improves the outcome
A practitioner-led pathway isn’t automatically better, but it is often more clinically coherent. It allows the test to sit inside a real differential process. That means someone is asking whether the stool findings fit the symptoms, whether food-related immune triggers are likely, whether histamine issues are muddying the picture, and whether any findings need GP review.
Direct-to-consumer testing can still be appropriate for informed patients. But convenience often comes with a trade-off. You may receive a report before you have a framework to interpret it.
If the provider sells certainty, be cautious. Good microbiome work is interpretive medicine, not fortune telling.
A practical standard to hold providers to
In my view, reputable providers do three things well. They explain the method clearly. They tell you what the test cannot answer. And they build their recommendations around clinical decisions rather than product bundles.
That same standard applies when stool testing is combined with blood-based diagnostics. For any complementary blood testing, pathology collection and clinical-grade serum analysis are preferable to casual home alternatives because pre-analytical handling affects reliability.
Preparing for Your Test and Collecting Your Sample
Preparation errors can reduce the value of an otherwise good test. That sounds obvious, but it’s one of the most common reasons people end up with results that are harder to interpret than they should be.
Before you collect the sample
Read the lab instructions in full before opening the kit. Different providers use different preservatives, containers, and transport requirements. Don’t assume one test works like the last one.
Also review any advice about antibiotics, antimicrobials, probiotics, or other supplements. Some providers ask for a pause before collection. Some don’t. You should only change medication or supplement use with practitioner guidance.
A simple checklist helps:
- Check timing first: Don’t collect when you’re about to travel or can’t ship promptly.
- Review restrictions carefully: Follow the provider’s instructions, not internet advice from another test brand.
- Label everything immediately: Most avoidable errors happen after collection, not during it.
During collection and return
The sample should be collected exactly as instructed, sealed properly, and returned within the required timeframe. Stool testing depends on sample integrity. If the sample is mishandled, delayed, or exposed to unsuitable temperatures, the result may become less reliable.
This short video gives a useful visual overview of a typical collection process:
Where clinical-grade process still matters
Even though most microbiome tests use stool samples collected at home, the principle is the same as any serious diagnostic work. Good results rely on good handling.
That’s also why, when blood testing is used alongside stool analysis, venous blood draw through pathology collection remains the better standard. Blood serum testing depends on professional collection, stability, and laboratory processing. If you’re building a full picture rather than buying isolated tests, the quality of the collection pathway matters almost as much as the assay itself.
How to Interpret and Action Your Microbiome Results
The biggest mistake people make after receiving a report is reading it like a morality chart. More green must be good. More red must be bad. Real interpretation isn’t that simple.
A microbiome report is better read as a pattern analysis. The clinically useful questions are whether diversity appears reduced, whether key groups are underrepresented, whether opportunistic organisms are overgrown, and whether those findings match the person’s symptoms.
What deserves attention in a report
Some findings matter more than others.
- Low diversity: This can suggest reduced resilience in the ecosystem.
- Low beneficial species or groups: This may fit symptoms linked to poor fermentation balance or reduced tolerance.
- Raised opportunists: This matters most when symptoms, history, and other markers support the finding.
- Inflammation or digestive markers: These often shape whether a result should stay in the wellness lane or be escalated for medical review.
An isolated result rarely justifies a full protocol by itself. Patterns do.
Turning findings into action
Most useful action plans fall into three categories.
Diet changes that are specific, not random
Dietary work should follow the report logic. If the pattern suggests poor resilience and low diversity, the answer is usually not a highly restrictive diet unless symptoms make that necessary in the short term. Over-restriction can leave patients eating fewer foods and feeling worse.
A practical approach often includes more diversity in tolerated plant foods, a gradual increase in fibre exposure where appropriate, and temporary avoidance of clear aggravators. The key word is tolerated. Pushing high-fibre strategies into an already reactive gut can backfire.
Lifestyle factors that alter the terrain
Microbes don’t exist separately from daily physiology. Sleep disruption, high stress load, irregular meals, and repeated antimicrobial exposure can all affect the pattern you see on a stool report.
Don’t ask a microbiome protocol to compensate for a lifestyle that keeps re-creating the same problem.
That’s why the best plans include stress regulation, meal regularity, and a realistic review of what the patient is repeatedly taking, including supplements that may be aggravating symptoms.
Supplements that match the report
Restraint helps. More products don’t equal better care. If a practitioner suggests probiotics, prebiotics, antimicrobials, or digestive support, the intervention should match the pattern rather than follow a generic gut stack.
For patients trying to understand the broad role of supplementation, this explainer on Prebiotics and Probiotics Supplements can help distinguish categories. For a gut-focused overview tied more closely to microbiome support, this article on prebiotics and probiotics for the gut microbiome adds helpful context.
When you should involve a practitioner
If the report suggests a pathogen, major inflammatory concern, severe symptom correlation, or repeated failure with self-directed interventions, bring the result to a GP or qualified practitioner. The goal isn’t dependence. It’s correct interpretation.
A report is only useful if it changes management safely. That may mean further stool work, medical review, dietary strategy, or complementary blood testing to identify ongoing triggers.
Building Your Full Health Picture The Integrated Clinical Pathway
A stool test can describe the state of the ecosystem. It often can’t fully explain the trigger that keeps disturbing it.
That’s the gap many patients notice after microbiome testing. They learn they have dysbiosis, reduced beneficial organisms, or a pattern consistent with inflammation, but they still don’t know why the problem persists. In practice, chronic symptoms often involve more than one layer.
The stool result shows the pattern. Blood serum testing can help explain the driver
One important missing piece can be food-related immune activation. In this context, clinical-grade IgG testing using venous blood serum may add value. A stool report might suggest a disrupted environment. A blood serum test can help identify whether specific foods are a plausible ongoing trigger in that person’s case.
This isn’t a replacement for microbiome analysis. It answers a different question. The stool test asks what the gut environment looks like. The blood serum test asks whether repeated exposure to certain foods may be contributing to the inflammatory background.
The same logic applies to DAO enzyme testing in patients with suspected histamine-related symptoms. If someone has bloating, flushing, headaches, skin symptoms, or reactivity that seems inconsistent, stool findings alone may not clarify whether impaired histamine handling is part of the picture.
A more practical sequencing strategy
For many patients with chronic but non-specific symptoms, the most useful pathway looks like this:
- Start with the symptom pattern and history. Decide whether the primary question is infection, dysbiosis, food-related reaction, or histamine-related intolerance.
- Choose the stool test type accordingly. Broad sequencing for ecosystem questions. Targeted PCR for defined suspects.
- Add clinical-grade blood serum testing when the stool result doesn’t explain the trigger. This is often where delayed food reactions or DAO issues become clinically relevant.
- Build one plan, not three separate protocols. If every test leads to an unrelated set of restrictions and supplements, the pathway isn’t integrated.
A helpful example of the broader gut-systemic connection appears in this discussion of the gut microbiome and rheumatoid arthritis. The key point isn’t that every patient has the same mechanism. It’s that isolated results can miss the full network driving symptoms.
The best diagnostic pathway reduces guesswork. It doesn’t increase the number of disconnected tests.
When stool findings, symptoms, and blood serum markers point in the same direction, treatment becomes much more precise. That’s where testing stops being interesting data and starts becoming clinically useful.
If you want a more complete pathway for ongoing bloating, fatigue, skin flare-ups, headaches, or suspected food-related symptoms, ImuPro Australia offers clinical-grade testing that can complement microbiome work. Their focus is on venous blood draw, pathology collection, and blood serum analysis, which helps distinguish clinical diagnostics from casual home-testing approaches. For patients who need more than a stool report alone, that added layer can help turn scattered clues into a more coherent plan.