A common first appointment starts like this. Someone has already removed dairy, then gluten, then a handful of other foods, yet the bloating, headaches, skin flares, or fatigue keep coming back without a clear pattern.
In practice, that is usually the point where guesswork has stopped being useful.
Food can be involved in chronic symptoms, but the method used to investigate it matters. Delayed reactions are difficult to track from memory alone because symptoms may appear well after the meal, overlap with other foods eaten that day, or sit alongside non-food factors such as stress, illness, medication, or poor sleep. That is why I prefer a clinical pathology pathway over broad self-experimentation or home collection kits.
The professional standard for food sensitivity testing in Australia uses venous blood serum collected through a pathology blood draw and analysed in a laboratory with established handling procedures. That approach does not promise a diagnosis on its own, and it should never replace medical assessment for coeliac disease, allergy, gastrointestinal disease, or other causes of ongoing symptoms. What it does provide is a more controlled starting point for investigation, with better sample quality and clearer accountability than finger-prick kits sent off from home.
That distinction matters early.
Patients often assume all food sensitivity tests are broadly the same. They are not. A venous sample collected through a pathology service gives the lab enough properly handled serum to run the assay under tighter collection and transport standards. If the goal is to make sensible diet changes based on the result, that extra rigour is worth it.
Navigating Chronic Symptoms and the Role of Food
Many people come in with the same story. Their symptoms are real, recurring, and disruptive, but routine changes haven't led to a clear answer. They may notice that certain meals seem to make things worse, yet the pattern isn't consistent enough to trust.
That lack of certainty is exactly why casual guesswork often fails. If symptoms are delayed, a food eaten today may affect you much later, and several foods may overlap across the same period. By then, individuals either remove too many foods or stop investigating altogether.
When food becomes a reasonable line of enquiry
Food isn't always the cause, but it becomes a sensible place to look when symptoms are persistent, unexplained, and repeatedly influenced by eating patterns. In practice, the most common concerns people raise include digestive discomfort, low energy, headaches, joint pain, and skin symptoms that fluctuate without an obvious trigger.
A useful approach is to treat food as one possible contributor, not the only explanation. That keeps the process balanced and reduces the risk of unnecessary restriction.
Practical rule: Test to guide decisions, not to confirm a fear. The goal is clarity, not a longer list of foods to avoid.
Why structure matters
A structured process does two things well. First, it separates delayed food sensitivity work from immediate allergy concerns. Second, it gives you a path from symptoms to action that isn't based on internet lists or broad elimination done without context.
For readers exploring food sensitivity testing australia, that structure usually includes:
- A clinical review to understand symptom timing, diet, and medical history
- A venous blood draw collected through a pathology setting rather than a home sample
- Laboratory analysis of blood serum using established methodology
- Interpretation with a practitioner so results are used sensibly
- A dietary plan that removes and reintroduces foods in a controlled way
The conversation becomes more useful. Instead of asking, “What food should I cut out?”, the better question is, “What pathway gives me the most reliable information to work with?”
Understanding Delayed Food Sensitivities
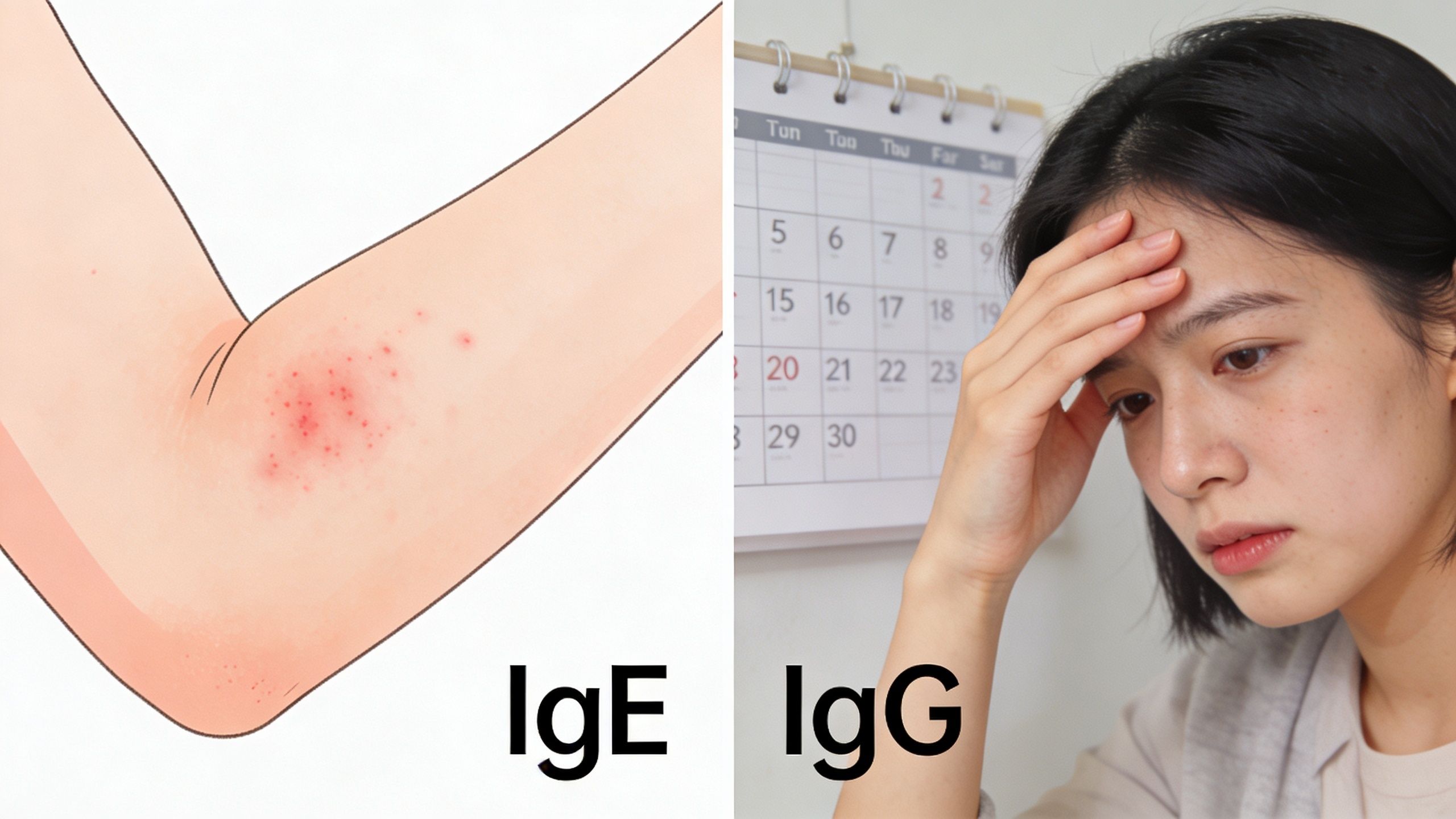
You eat dinner on Monday, feel reasonably well, then wake on Wednesday with bloating, a headache, and skin irritation. That pattern does not fit the classic picture of an immediate food allergy, and it is one reason delayed food sensitivity work can become relevant in clinic.
An IgE-mediated allergy usually causes symptoms quickly and can be medically urgent. A delayed IgG-related food sensitivity refers to a different immune pattern, where symptoms may appear well after the food was eaten and may be less specific. That time lag is exactly why people often struggle to connect symptoms to the right food.
Why delayed reactions are hard to spot
In practice, delayed symptoms can show up hours to days after exposure. By that point, several meals may have passed, ingredients may have repeated across different foods, and a diary can point you in the wrong direction.
This is one reason I advise patients not to rely on symptom guessing alone.
Food diaries still have value. They help identify patterns, portion size, frequency, and overlap with stress, sleep, alcohol, travel, or medication use. But for delayed reactions, diary data is often more useful when paired with a pathology-based testing process rather than used as the whole investigation. If you want a plain-language overview of that pathway, this guide on how to test for food intolerance through a clinical process is a useful starting point.
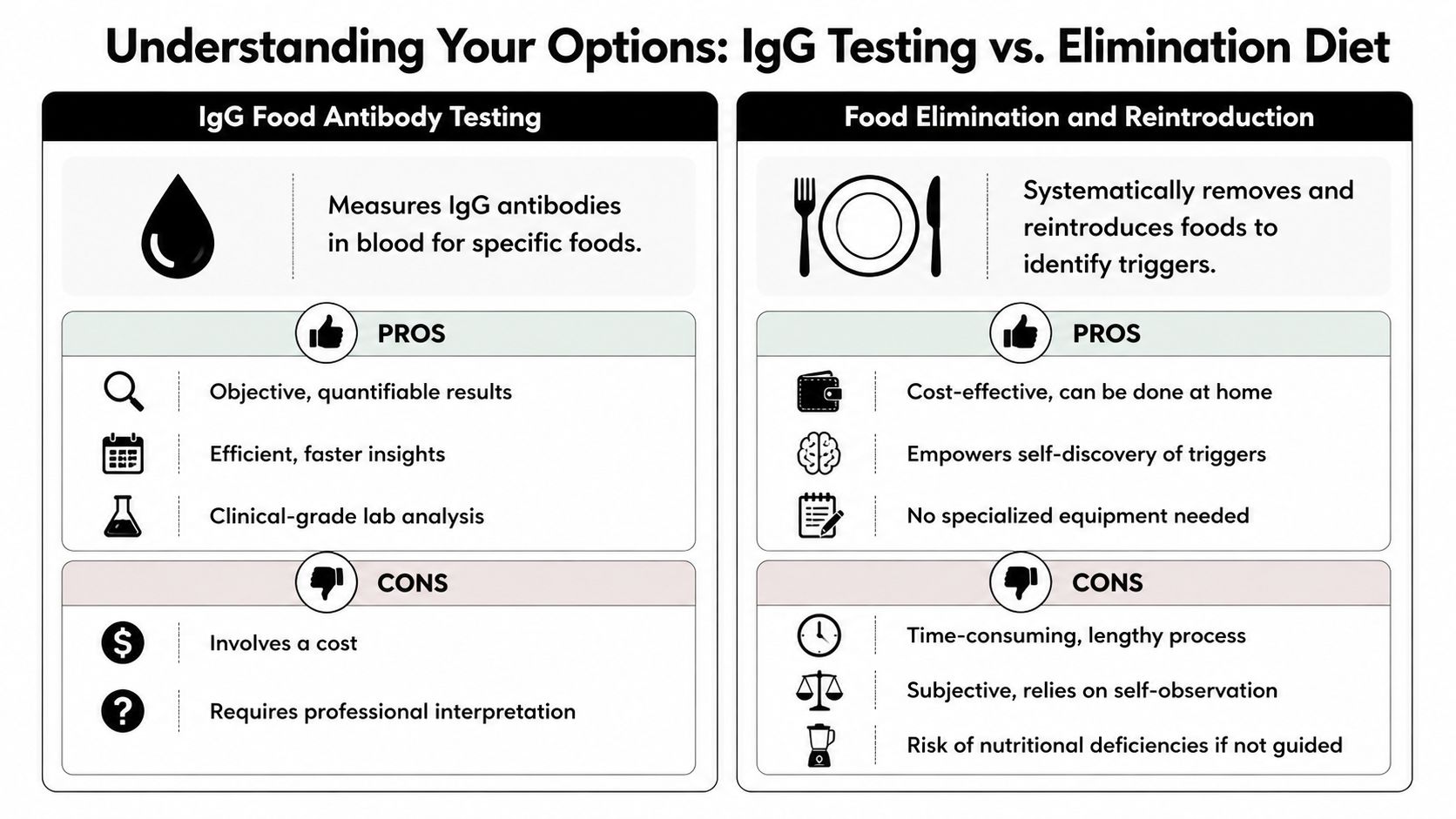
What IgG testing is and is not
IgG food antibody testing is a clinical support tool. It is not a stand-alone diagnosis, and it should not be used to generate a long list of permanent food exclusions without review.
That distinction matters.
Used well, results can help prioritise which foods deserve a structured elimination and reintroduction trial. Used poorly, they can lead to unnecessary restriction, anxiety around eating, and diets that become harder to maintain than the original symptoms.
The method also matters. For this type of investigation, venous blood collection through a pathology setting gives a cleaner and more controlled sample than home collection kits. That does not make interpretation simple, but it does improve the quality of the specimen being analysed and reduces avoidable pre-analytical problems.
Why the clinical pathway matters
Many people looking into food sensitivity testing australia have already tried online symptom checkers, broad elimination diets, or direct-to-consumer kits. The problem is not just convenience versus inconvenience. The problem is reliability.
A professionally collected venous blood sample follows the same pathology principles used across many other forms of laboratory medicine. Patient identification, sample handling, transport conditions, serum preparation, and laboratory processing are controlled. Those steps affect result quality. Home kits can fall short before the sample even reaches a lab, which makes interpretation harder and confidence lower.
Delayed food sensitivity testing is most useful when the question is practical. Which foods should be trialled first, under supervision, to see whether symptoms improve?
Why some patients still explore this route
Immediate allergy testing does not explain every food-related complaint seen in practice. Some patients have recurring symptoms that clearly seem connected to eating, yet standard allergy assessment does not account for the full picture. In that setting, delayed sensitivity testing may help guide the next stage of investigation, provided the results are interpreted conservatively and followed by real-world dietary testing.
The goal is not to prove that food is always the cause. The goal is to use a higher-standard clinical pathway to decide whether certain foods are worth testing in a structured, sensible way.
Clinical Food Sensitivity Testing Methods Explained
Once delayed reactions are on the table, the next question is which clinical tools are worth considering. In practice, two blood-based pathways often come up. One looks at IgG food antibodies. The other looks at DAO enzyme status when histamine intolerance is a concern.
They don't measure the same thing, and they shouldn't be used interchangeably.
IgG food antibody testing
IgG food antibody testing in Australia uses indirect ELISA, a reproducible laboratory method that measures antibody responses in blood serum. In Australian practice, these panels may range from 96 to 270 foods, depending on the provider and panel design, and some advanced protocols also assess immune complexes involving complement marker C3d (Australian clinical summary of ELISA food antibody testing).
This method is designed to support investigation of delayed immune responses rather than immediate allergic reactions. It can be relevant when symptoms are broad, recurring, and hard to link to one obvious trigger.
An important limitation is often overlooked. Pre-test dietary exposure matters. If you've been avoiding many foods before the blood draw, the test may produce false negatives because there may not be enough circulating antibodies to detect. Clients need to be eating a reasonable variety of the foods being tested in the lead-up to collection.
For a practical overview of how that testing pathway works, this guide on how to test for food intolerance outlines the blood-based process in plain language.
DAO enzyme testing for histamine-related symptoms
DAO testing asks a different question. It doesn't map reactivity to a long food panel. Instead, it looks at the enzyme pathway involved in histamine breakdown. This can be relevant when symptoms appear to cluster around histamine-rich or histamine-liberating foods.
Typical complaints in that pattern may include digestive symptoms, flushing, headaches, skin symptoms, or a sense that reactions are inconsistent but often linked to aged, fermented, or highly processed foods. The value of DAO testing is that it narrows the investigation to a specific biological mechanism rather than treating every reaction as a broad food sensitivity issue.
A side-by-side view
| Test pathway | What it measures | Best suited to | Main limitation |
|---|---|---|---|
| IgG food antibody testing | IgG responses to selected foods in blood serum | Delayed, multi-food symptom patterns | Needs professional interpretation and enough recent dietary exposure |
| DAO enzyme testing | DAO-related histamine handling | Suspected histamine intolerance pattern | Doesn't identify broad food-specific IgG reactivity |
One example of a clinical-grade option
One blood-serum option available in Australia is ImuPro Australia, which offers panels such as Screen 22/44, Basic 90, Vegetarian 90 or Vegetarian+221, and Complete 270, with samples collected through local pathology centres and analysed using ELISA in an ISO-certified laboratory. That's a clinical testing pathway, not a general wellness kit.
The right test is the one that matches the mechanism you are investigating. Broad symptoms may justify an IgG panel. A histamine pattern may justify DAO assessment. Some people need one. Some need neither.
The Pathology-Grade Testing Process from Start to Finish
The quality of a food sensitivity test doesn't start in the lab. It starts with how the sample is collected. If the collection process is weak, convenience-driven, or poorly controlled, the result becomes harder to trust.
That's why a pathology-based pathway matters.
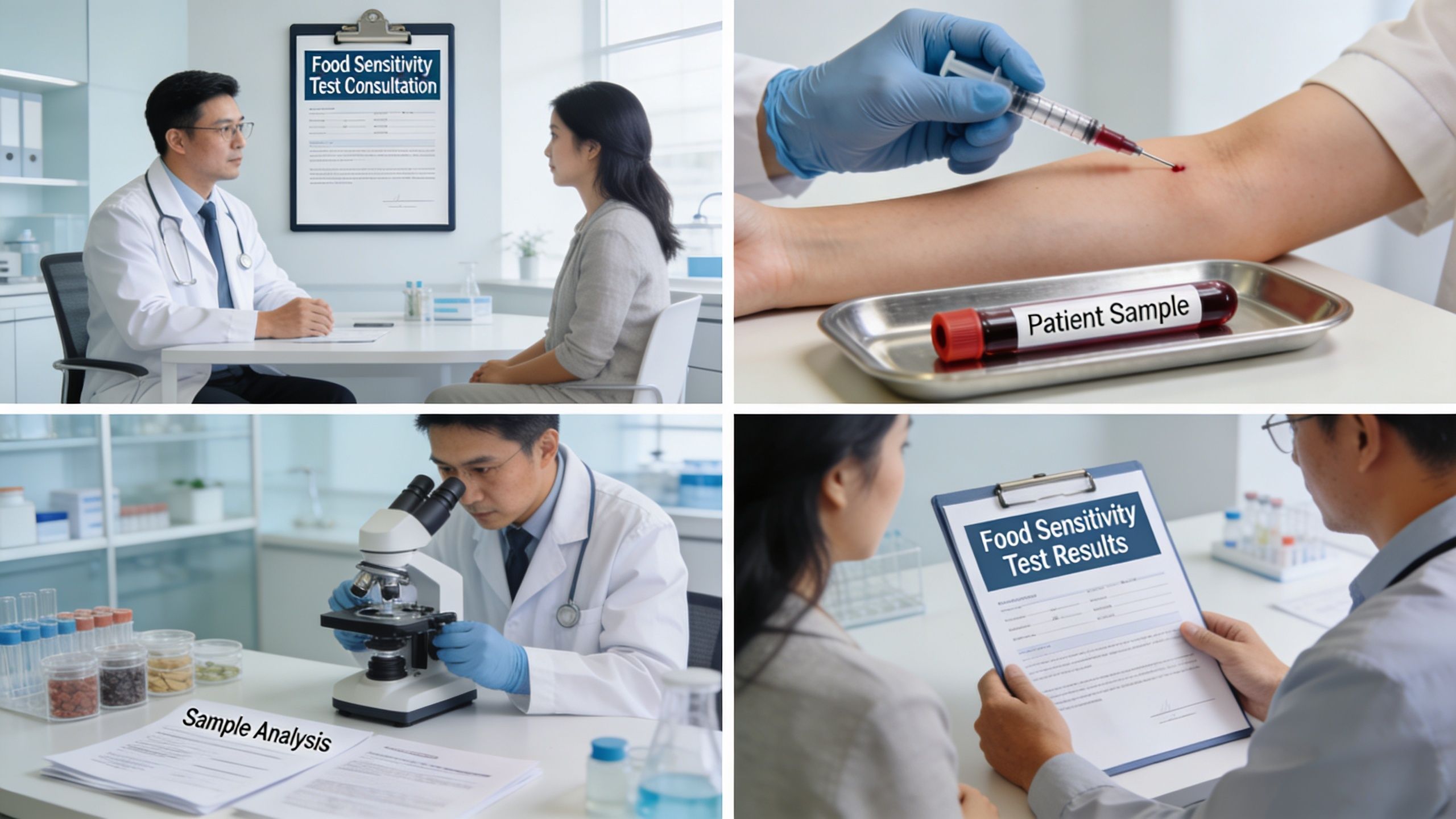
Step one brings the symptoms into focus
The process should begin with a proper review of your symptoms, diet, relevant history, and current exclusions. If you've already removed half a dozen foods, that needs to be known before testing because it can affect what the blood work can detect.
This conversation also helps decide whether food sensitivity testing is even the right next step. Sometimes a symptom pattern points more strongly toward digestive dysfunction, a food chemical issue, or a broader medical problem that needs separate assessment.
Step two uses venous blood serum, not convenience sampling
A venous blood draw at a pathology collection centre is the benchmark for this kind of testing. It provides a controlled sample, proper handling, and a clear chain from collection through to laboratory analysis.
That matters because the Australian market includes both clinically validated blood-based testing and non-validated methods. The Australasian Society of Clinical Immunology and Allergy notes that methods such as hair analysis and bioresonance have been found to be inaccurate and unreliable, which is why established laboratory methodology and accredited processing are so important (ASCIA guidance on food intolerance testing and unreliable methods).
A pathology collection pathway also supports sample stability. In practical terms, that reduces avoidable variability and gives the lab a specimen that is suitable for serum analysis.
Step three is laboratory analysis under clinical controls
After collection, the serum goes to a laboratory using established analytical methods such as ELISA. Depending on the provider, turnaround for serum IgG testing in Australia can be 12 to 15 business days or, in some pathology-based settings, 10 to 20 days. The exact timeline matters less than the quality controls around processing and reporting.
Look for signs that the provider uses certified systems and recognised laboratory standards, not just attractive branding.
Before you see how reporting works in practice, this video gives a useful overview of the clinical testing pathway:
Step four turns a report into a plan
A good report doesn't list reactive foods. It groups results clearly, supports interpretation, and helps build an elimination and rotation strategy that still preserves dietary variety.
That final part is where many people need professional help. The report is data. The diet is the intervention. If those two aren't connected carefully, even a technically sound test can lead to an unhelpful outcome.
How to Choose a Reputable Testing Provider in Australia
Not all providers in food sensitivity testing australia are working to the same standard. Some operate through clinical pathways. Others package weak methods as if they are equivalent. They aren't.
The easiest way to reduce risk is to judge the provider by its process, not its marketing.
The checklist that matters
When I review a testing option, these are the points that deserve attention first:
- Venous pathology collection. If the provider doesn't use a proper blood draw through a pathology setting, I would question the entire pathway.
- Blood serum analysis. The report should be based on serum processed by a clinical laboratory, not an indirect consumer shortcut.
- Established methodology. ELISA matters because the method itself is reproducible and widely used in clinical testing environments.
- Laboratory accreditation and quality systems. A provider should be clear about where the sample goes and under what standards it is processed.
- Interpretation support. A long list of reactive foods without context isn't helpful.
- A practical follow-up plan. The provider should explain how results are meant to guide elimination and reintroduction, not just deliver a coloured chart.
What should make you cautious
Some methods should be a clear warning sign. If a provider leans on hair analysis, bioresonance language, or broad claims without explaining the laboratory pathway, that's not a small issue. It's a methodological one.
A useful consumer guide on low-quality food intolerance tests outlines the kinds of warning signs that often separate clinical-grade testing from weaker alternatives.
If a provider can't explain sample collection, lab methodology, and how results are applied, they haven't earned your trust yet.
The trade-off to accept
A reputable provider may be less convenient than a wellness kit. There may be a referral step, a pathology appointment, and a waiting period for proper analysis. That's the price of rigour.
For many, that's a worthwhile trade. When symptoms have been persistent for a long time, the aim shouldn't be the fastest result. It should be the most clinically usable one.
Creating Your Post-Test Dietary Action Plan
Testing is only useful if it changes what you do next. A result on its own doesn't improve symptoms. The value comes from a structured elimination and rotation plan based on the foods that appear most relevant.
That matters in Australia because food-related concerns are common. The NSW Food Authority reports that up to 25% of Australians believe they have a food intolerance, while hospital admissions for severe allergic reactions have surged by more than 350% in two decades. It also notes that allergies affect about 2 in 100 adults, while intolerances are more prevalent, which is why structured dietary management is so important (NSW Food Authority information on allergy, intolerance and dietary management).
What an elimination and rotation plan actually does
The usual next step is to temporarily remove the foods showing the strongest reactivity, while keeping the overall diet as nutritionally broad as possible. This isn't meant to become a permanent restricted diet by default.
Then comes the rotation phase. Instead of relying heavily on the same substitute foods every day, you vary tolerated foods to reduce repetition and make the diet more balanced.
A practical sequence
Prioritise the highest concerns
Start with the foods most likely to matter, based on the report and your symptom history.Keep the plan time-limited and supervised
Broad restriction without review can create confusion and unnecessary fear around eating.Track symptom changes carefully
Look for consistent patterns, not one-off fluctuations.Reintroduce in a deliberate order
Foods are usually challenged one at a time so you can assess tolerance more clearly.Refine rather than over-restrict
The end point isn't to avoid everything reactive forever. It's to identify what your body handles, what it doesn't, and in what amount.
For readers wanting help interpreting the reporting side, this article on IgG food sensitivity test results explained gives a practical overview.
A useful post-test plan is specific enough to test a hypothesis, but flexible enough to preserve nutrition, variety, and quality of life.
What tends to work better than guesswork
The patients who do best usually avoid two extremes. They don't ignore the results, and they don't panic over them. They use the report as a map, then let reintroduction confirm what is clinically meaningful.
That's the point of the whole process. Testing narrows the field. The diet confirms what matters.
Taking the Next Step Towards Better Wellbeing
Food sensitivity work is most helpful when it's grounded in the right question. Are you dealing with an immediate allergic reaction, a delayed immune pattern, a histamine issue, or something else entirely? Once that question is clearer, the testing pathway becomes easier to choose.
The practical standard is straightforward. If you're considering food sensitivity testing australia, look for a pathway built around venous blood serum, pathology collection, and clinical-grade laboratory analysis. That gives you a much stronger foundation than methods that prioritise convenience over sample quality.
It's also worth keeping your expectations realistic. An IgG report doesn't replace clinical reasoning, and it doesn't excuse a poorly planned restrictive diet. Its value lies in helping you make a more focused elimination and reintroduction plan, with less guesswork and better structure.
For many people, that shift alone is significant. Instead of reacting to symptoms meal by meal, you move into a process that is organised, evidence-aware, and easier to act on. That doesn't solve everything overnight, but it does give you a clearer way forward.
If you're ready to explore a clinical pathway, ImuPro Australia provides blood-serum IgG food sensitivity testing and DAO testing collected through local pathology centres, with reports designed to support a structured elimination and rotation plan.