You’ve had the blood tests. You’ve tried cutting out one food, then another. You’ve been told everything looks “normal”, yet the bloating keeps returning, your energy dips by mid-afternoon, your skin flares without warning, or your head feels foggy for no clear reason.
That experience is common in people who start looking into functional medicine doctors. They’re often not searching for something exotic. They’re looking for a clearer explanation. They want to know why symptoms persist when routine checks haven’t given them a useful answer.
For many people, the confusion deepens when food seems involved but standard allergy testing doesn’t explain the pattern. Symptoms may appear hours or days later, which makes the trigger hard to spot. In cases like that, broader context can help, including how gut function, immune activity, stress, sleep, and diet interact. That’s also why some readers find IPA's insights on diet in psychiatric care useful. It shows how nutrition can affect more than digestion alone, including mood and cognitive function.
If your symptoms seem scattered across different body systems, learning more about the gut-immune connection can also help frame the bigger picture. A practical starting point is what your gut microbiome reveals about your health, especially if digestive issues sit alongside fatigue, headaches, or skin changes.
Beyond Symptoms An Introduction to Functional Medicine
Functional medicine starts with a different question. Instead of asking only, “What condition fits these symptoms?”, it asks, “What processes may be driving them?”
That shift matters when symptoms are long-standing, change over time, or affect several systems at once. A person might have reflux, alternating bowel habits, poor concentration, and joint discomfort. In a standard short consultation, each issue can look separate. In a functional medicine consultation, they may be investigated as connected parts of the same pattern.
Why the root cause idea matters
A useful way to think about it is this. Symptoms are often the body’s signal lights, not the whole story. If the signal keeps flashing, dimming the light doesn’t always solve the problem underneath.
Functional medicine doctors usually look at factors such as:
- Dietary patterns: what you eat, how often, and whether symptoms follow certain foods
- Digestive function: bowel habits, bloating, reflux, gut infections, or signs of poor tolerance
- Stress load: ongoing stress can affect sleep, appetite, gut motility, and immune regulation
- Sleep quality: not just hours slept, but whether sleep feels restorative
- Environmental and family context: medications, exposures, life events, and inherited tendencies
Functional medicine doesn’t replace emergency medicine or specialist care. It’s a framework for investigating persistent, multifactorial problems more thoroughly.
When people usually seek this kind of care
Many people turn to functional medicine doctors after a cycle of partial answers. They may receive symptom-based treatment that helps for a while, but the issue keeps returning. Others want a more personalised explanation of how food, lifestyle, and biology are interacting in their own case.
That doesn’t mean every symptom has a hidden food trigger or a single neat cause. Often, chronic symptoms come from several contributors layered together. Functional medicine is built around teasing those layers apart in a structured way.
What Are Functional Medicine Doctors
A person with long-running fatigue, bloating, headaches, and poor sleep may have seen several clinicians and still feel as though the pieces do not fit together. A functional medicine doctor aims to build that full picture. The role is not merely to label symptoms, but to examine how multiple body systems may be interacting and why those patterns keep repeating.
Functional medicine doctors are licensed clinicians who use a patient-centred, systems-based method to assess chronic or recurring health concerns. They look across digestive function, immune activity, hormone signalling, metabolism, sleep, stress physiology, medications, diet, and environmental exposures. In practice, that means asking how one problem may be influencing another. Poor sleep can affect blood sugar regulation. Ongoing gut irritation can affect nutrient absorption. Chronic stress can alter digestive motility, appetite, and inflammatory signalling.
A useful way to understand their role is to picture a mechanic tracing an electrical fault in a car. The warning light on the dashboard matters, but it is only the starting point. The essential work is finding which circuits are misfiring, what triggered the problem, and which test will confirm it.
A different clinical lens
Conventional medicine remains the standard for acute illness, infection, injury, surgery, and disease that needs urgent treatment. Functional medicine is often used for a different clinical problem. It is most relevant when symptoms are persistent, involve several systems at once, or have not responded fully to symptom-based care.
The difference is not only philosophy. It is also method. A legitimate functional medicine doctor should use the same clinical discipline expected in other areas of healthcare: careful history-taking, physical assessment where appropriate, and diagnostics with known clinical utility.
That point matters because the term "functional medicine" is sometimes confused with general wellness advice, supplement sales, or home kits with uneven accuracy. Good care is more grounded than that. When laboratory testing is needed, higher-quality practices often rely on clinically supervised assessment and medical-grade diagnostics, including venous blood draws where accuracy, sample stability, and interpretation matter. That is especially relevant for markers affected by timing, specimen handling, and lab methodology.
How functional medicine compares to conventional care
| Aspect | Conventional Medicine | Functional Medicine |
|---|---|---|
| Primary focus | Diagnose disease and manage symptoms | Investigate contributors to ongoing symptoms and dysfunction |
| View of the body | Often organised by organ system or specialty | Examines how systems influence one another |
| Typical consultation style | Shorter, problem-focused visits | Longer history-taking with more context on triggers, timelines, and patterns |
| Diagnostic focus | Standard pathology, imaging, acute findings, disease thresholds | Standard pathology plus targeted testing selected to answer a clear clinical question |
| Treatment goal | Relieve symptoms, treat disease, prevent progression | Improve function by addressing identifiable drivers where evidence supports action |
| Patient role | Follows a treatment plan | Tracks symptoms, responses, and day-to-day factors that affect recovery |
Testing is one area where readers often get confused, so it helps to be direct. Functional medicine should not mean ordering every available panel or relying on low-accuracy home testing. Good clinicians choose tests for a reason, explain what each result can and cannot show, and connect those findings back to symptoms, history, and standard medical care.
For readers trying to identify clinicians who work in this model, ImuPro Australia maintains a directory of recommended functional medicine practitioners that includes practitioners using functional medicine principles.
Practical rule: A functional medicine doctor should be able to explain what they are testing, why that test was chosen, how reliable it is, and how the result would change your care.
Conditions Commonly Addressed With Functional Medicine
A common pattern looks like this. Someone books an appointment for bloating or reflux, but the full story also includes fatigue, headaches, skin flares, poor sleep, or a sense that meals leave them feeling worse instead of better. Symptoms that seem unrelated often travel together.
Digestive complaints that won’t settle
Digestive symptoms are one of the most common reasons people seek this kind of care. Bloating, abdominal discomfort, reflux, irregular bowel habits, and feeling unwell after eating can point to several different mechanisms, not one single diagnosis.
That distinction matters. The gut is not just a food tube. It also helps regulate nutrient absorption, immune activity, and chemical signalling between the digestive tract and the brain. If digestion is disrupted for long enough, the effects can show up far beyond the bowel.
This is also where legitimate functional medicine separates itself from wellness marketing. A careful clinician does not guess from symptoms alone or rely on a low-accuracy home kit to explain every food reaction. They may use standard investigations and, where appropriate, targeted clinical-grade testing such as venous blood draws to check whether a suspected trigger is plausible.
Skin, headaches, and other symptoms that seem disconnected
Patients are often told their skin, sinuses, headaches, and digestion must be separate issues because they involve different body parts. In practice, the body does not work in isolated compartments. The immune system, gut lining, nervous system, and inflammatory pathways constantly exchange signals.
A useful comparison is a house with one faulty circuit affecting lights in different rooms. The kitchen, bedroom, and hallway bulbs may flicker in different ways, but the wiring problem can still be shared. In the same way, one driver can contribute to symptoms in several places.
A person might notice:
- Skin changes: eczema-like irritation, flushing, or acne flare-ups
- Head symptoms: headaches after meals, brain fog, poor concentration
- Body-wide discomfort: aches, stiffness, or a persistent inflamed feeling without a clear explanation
These patterns do not prove a single cause. They do suggest that a broader clinical workup may be more useful than treating each symptom as a separate mystery.
Fatigue, hormonal shifts, and ongoing immune strain
Fatigue is another frequent reason people look for answers outside a brief symptom-based appointment. Low energy can reflect poor sleep, unstable blood sugar, under-fuelling, chronic inflammation, digestive problems that affect absorption, or a prolonged stress response. Hormonal symptoms can sit in the same picture rather than in a separate one.
Functional medicine doctors often assess patterns such as:
- Fatigue with brain fog: explored in the context of sleep quality, food intake, digestion, and inflammatory load
- Hormonal irregularity: menstrual changes, PMS, peri-menopausal symptoms, or thyroid-related complaints
- Recurring immune-type symptoms: symptom clusters that flare, settle, and return without an obvious short-term explanation
The goal is not to label every ongoing symptom as complex or hidden. The goal is to identify which complaints belong together, which need conventional medical investigation first, and where higher-quality diagnostics can clarify the next step. That is why credible functional medicine depends so heavily on careful history, standard medical reasoning, and testing that is accurate enough to guide real decisions.
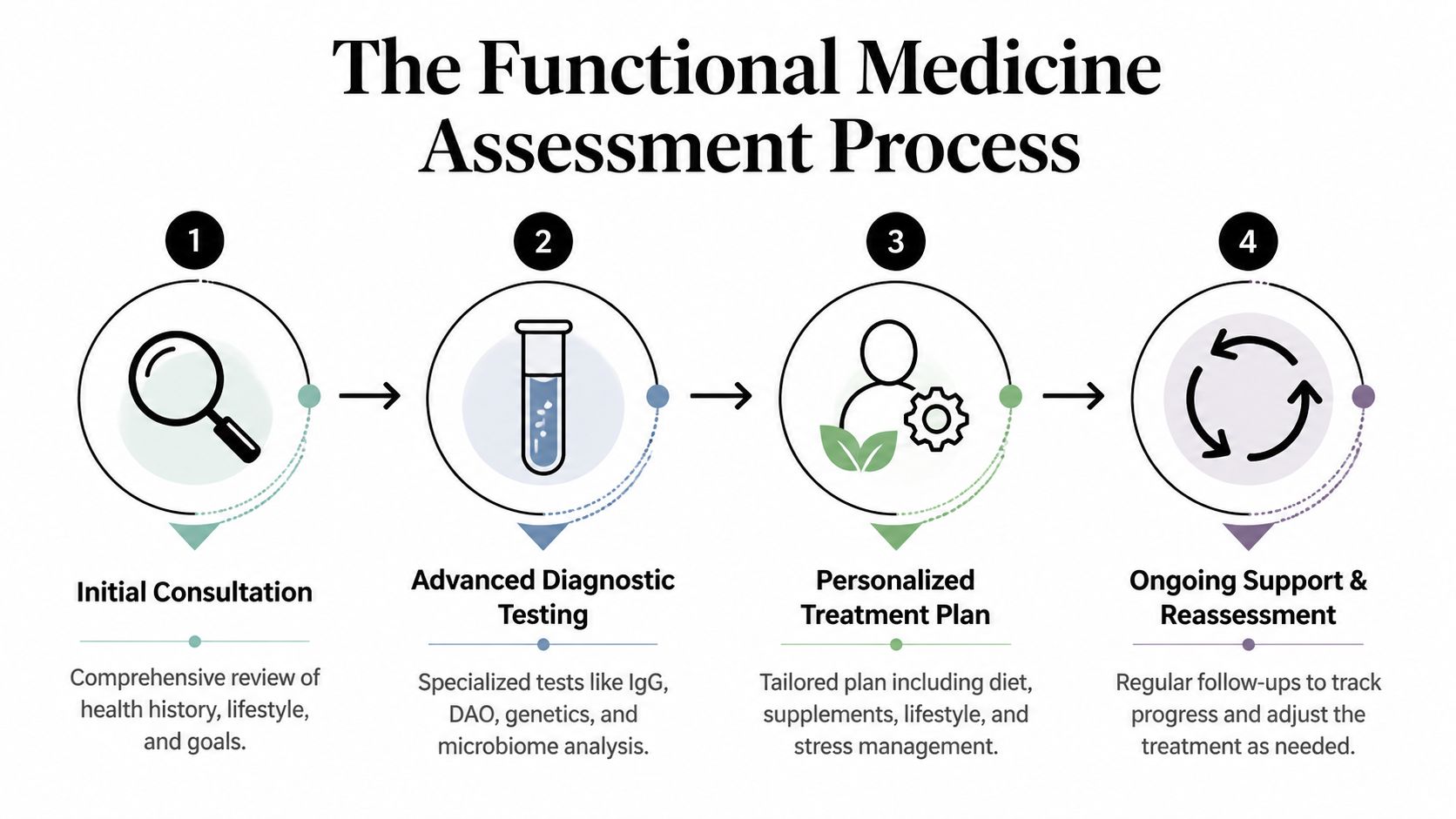
The Functional Medicine Assessment Process
You sit down for an appointment about bloating, fatigue, headaches, and broken sleep, and within a few minutes it becomes clear that none of those symptoms can be understood in isolation. A careful functional medicine assessment works more like assembling a case history than ticking boxes on a form. The clinician is looking for sequence, triggers, and links between body systems that may seem unrelated on the surface.
Step one is building a timeline
The first consultation is usually detailed because timing changes meaning. Fatigue that began after a viral illness raises different questions from fatigue that appeared after months of poor sleep, restrictive eating, or chronic reflux. The clinician may ask about childhood health, antibiotics, infections, travel, bowel habits, skin changes, menstrual history, medications, exercise, stress, and how symptoms shift around meals.
That level of detail helps turn a loose collection of complaints into a pattern.
A timeline often reveals the first domino. Symptoms may cluster after pregnancy, a stressful period, repeated antibiotic use, a major diet change, or a long stretch of overwork. Without that sequence, it is easy to chase each symptom separately and miss the mechanism connecting them.
Testing should solve a specific problem
Useful testing starts with a clinical question. Are symptoms pointing toward inflammation, nutrient depletion, blood sugar instability, digestive dysfunction, or a food-related immune pattern? A legitimate assessment uses tests to clarify those questions, not to generate a stack of results with no clear action.
Common next steps may include:
- Blood-based assessment: markers related to immune activity, nutrient status, metabolism, and other medically relevant patterns
- Digestive investigation: selected when the history suggests malabsorption, altered bowel function, or gut-related symptom triggers
- Targeted follow-up testing: used when the story points toward delayed food reactions or histamine breakdown issues
People comparing options often find it helpful to read the difference between allergy and intolerance testing before they book, especially if food seems involved. This guide to allergy and intolerance test options gives useful context for that discussion.
Why clinical-grade sample collection matters
Quality control distinguishes medical assessment from wellness marketing.
For markers such as IgG antibodies or DAO enzyme activity, the sample itself matters almost as much as the laboratory method. Venous blood drawn through a pathology collection centre gives a controlled starting point. Serum is collected, stored, transported, and processed under conditions designed to reduce pre-analytical error.
A home kit may sound convenient, but convenience is not the same as accuracy. If a sample is poorly collected, exposed to temperature swings, delayed in transit, or handled inconsistently, the final result becomes harder to trust. That is a serious problem if the test is being used to guide dietary restriction, further investigation, or treatment decisions.
A useful analogy is a blood pressure reading. One number taken with the wrong cuff size, in the wrong position, tells you much less than a properly performed measurement in clinic. Functional medicine testing works the same way. Better collection standards produce results that are safer to interpret in a real clinical context.
The plan usually unfolds in stages
Once the history and diagnostics are in place, the practitioner builds a staged plan instead of changing everything at once. That makes it easier to tell what is helping, what is neutral, and what may be making symptoms worse.
A staged plan often includes:
- Removing likely triggers: for example, foods, habits, or exposures that match the symptom pattern
- Supporting core physiology: sleep, meal structure, bowel regularity, stress regulation, and nutrient repletion
- Reviewing response over time: using symptoms, follow-up history, and selected retesting where appropriate
This kind of process is one reason some patients experience meaningful improvement with functional medicine care. That does not mean every person responds the same way. It means the model, when grounded in careful history, clinical reasoning, and high-quality diagnostics such as venous blood collection, can produce a clearer and more evidence-based path forward.
Understanding Key Diagnostic Tools IgG and DAO Testing
A common pattern in clinic goes like this. Someone eats reasonably well, has already tried cutting out a few obvious trigger foods, and still deals with headaches, bloating, flushing, sinus symptoms, or itchy skin that seem to appear without a clear cause. The problem is not always a classic allergy. Sometimes the question is less about an immediate immune alarm and more about whether the body is reacting repeatedly, or struggling to break down compounds such as histamine.
IgG is not the same as an IgE allergy
IgE allergy testing looks for the type of reaction people often recognise straight away. Hives, swelling, wheeze, and rapid symptoms after exposure fit that picture.
IgG food testing asks a different question. It examines whether certain foods are associated with a delayed immune response pattern that may be contributing to ongoing symptoms over time. A useful way to understand the difference is this. IgE acts more like a fire alarm. IgG is closer to repeated friction. It may not create an immediate emergency, but it can still matter if the same exposure keeps aggravating an already stressed system.
Interpretation needs care. A high IgG result does not automatically mean a food is harmful, and it should not be used in isolation to create a long list of permanent food exclusions. The result becomes useful when a clinician compares it with your symptom timeline, dietary pattern, and response to a structured elimination and reintroduction plan.
Why specimen quality matters
The quality of the sample shapes the quality of the answer. For IgG analysis, a venous blood draw processed as serum gives the laboratory a controlled specimen with standard handling conditions. That is very different from treating testing as a casual wellness purchase.
This distinction matters. If a result may influence diet changes, supplement decisions, or further medical investigation, the collection method should match the seriousness of the decision. Clinical pathology processes reduce avoidable errors in sampling, storage, and transport. Home collection kits can be convenient, but convenience is not the same as analytical reliability.
One example used in clinical discussion is ImuPro’s allergy and intolerance test information, which outlines how IgG-based food testing can be used as part of a broader assessment rather than as a stand-alone answer.
Where DAO testing fits
DAO stands for diamine oxidase, an enzyme involved in breaking down histamine, especially from food. If DAO activity is lower than expected, histamine can build up faster than the body clears it. The result can look confusing because the symptoms are spread across several body systems. A person may notice flushing, headaches, nasal congestion, gut discomfort, palpitations, or feeling worse after leftovers, fermented foods, wine, or other histamine-rich meals.
This is one reason DAO testing can add useful context. It helps the clinician examine whether the problem is only about a specific food, or whether histamine handling itself may be part of the picture. That distinction changes the plan. A person reacting to scattered high-histamine foods needs a different strategy from someone reacting to one or two clear dietary triggers.
How clinicians use the results
Good functional medicine does not stop at a lab report. The testing is there to sharpen clinical reasoning.
A thoughtful practitioner may use IgG and DAO findings to guide:
- A time-limited elimination plan: focused on the foods most likely to be relevant
- Careful reintroduction: to see whether symptoms return in a predictable way
- Histamine-aware dietary changes: if the history and DAO result point in that direction
- Follow-up review: to check whether the plan is helping daily function, not just changing numbers on paper
Patients usually find this process easier when the reasoning is explained clearly and the plan is practical. That communication is part of what helps improve patient experience in healthcare. In functional medicine, clear explanation matters because the goal is not just to identify abnormal markers. It is to connect accurate, clinical-grade testing with decisions that help the person in front of you.
How to Choose a Practitioner and Prepare for Your Visit
Choosing among functional medicine doctors takes a bit more thought than picking the nearest clinic. The right fit isn’t just about credentials. It’s also about method. You want someone who can investigate chronic symptoms carefully, explain their reasoning clearly, and use testing in a disciplined way.
What to look for
Start with basic professional grounding, then move to how the practitioner works.
- Clinical qualifications: Look for a practitioner with recognised health training and clear scope of practice.
- Experience with chronic patterns: Ask whether they commonly work with digestive symptoms, fatigue, skin issues, headaches, or histamine-related complaints.
- A clear testing philosophy: They should be able to explain why a test is being ordered and how the result will change management.
- Collaborative communication: Good practitioners teach as they go. You shouldn’t leave more confused than when you arrived.
Patient experience matters here as well. Much of what makes a consultation useful comes down to communication, follow-through, and clarity. Broader thinking on how clinics improve patient experience in healthcare can help you recognise the signs of a well-run service.
Questions worth asking before you book
A short call or email exchange can save a lot of frustration. Useful questions include:
- How do you approach chronic symptoms that cross multiple systems?
- When do you recommend venous blood draw testing through pathology collection?
- How do you interpret IgG or DAO results within the full clinical picture?
- What does follow-up look like after the first appointment?
- Do you work with patients remotely if they live outside major cities?
Finding a practitioner can be difficult outside metropolitan areas. A 2024 survey found that 62% of respondents in rural NSW and QLD struggled to locate certified practitioners, according to the verified data tied to this Restart Med reference. That’s one reason telehealth has become an important access point for regional patients.
For a useful overview of what a consultation can feel like in practice, this short video gives additional context.
How to prepare so the visit is more useful
The most productive first visit usually involves some preparation. Bring pattern, not just paperwork.
- Create a symptom timeline: note when problems began, major flares, and any obvious triggers
- Keep a food and symptom journal: especially if symptoms are delayed and hard to connect
- Gather prior results: blood work, scans, specialist letters, medication history
- List your goals: for example, less bloating, clearer skin, steadier energy, fewer headaches
Bring your observations, even if they seem messy. Functional medicine often starts by turning messy patterns into something clinically useful.
Your Path to Regaining Wellbeing
If you’ve been living with symptoms that don’t make sense, it helps to know there’s a structured way to investigate them. Functional medicine doctors work from the idea that chronic symptoms are often connected, even when they show up in different parts of the body.
That approach is most useful when it stays grounded in clinical reasoning. A detailed history matters. So does careful interpretation. And when testing is needed, the strongest path is usually one built on clinical-grade diagnostics and venous blood draw collection through pathology centres, not convenience-led shortcuts.
For many people, progress starts when the question changes from “How do I suppress this symptom?” to “What is my body responding to, and why?” That shift can turn scattered clues into a coherent plan.
You don’t need to arrive with all the answers. You do need a practitioner who knows how to investigate the right questions, and a process that treats your symptoms as meaningful signals rather than isolated annoyances.
If you’re exploring whether delayed food reactions or histamine-related patterns may be contributing to persistent symptoms, ImuPro Australia provides clinical-grade blood serum testing collected through pathology centres, with reporting designed to support discussion with your healthcare practitioner.