If you're looking at a bloodtype test kit, there’s a good chance you want more than trivia. Those inquiring about these kits often have motivations beyond casual interest. They’re frequently trying to make sense of ongoing bloating, fatigue, headaches, skin flare-ups, or a general sense that something in their diet isn’t agreeing with them.
That’s an understandable place to start. A home kit feels simple, private, and fast. You prick your finger, wait a few minutes, and get an answer that seems concrete. The problem is that a blood type result can only answer one narrow question. It tells you your ABO group and Rh status. It doesn’t tell you why you feel unwell after meals, why symptoms come and go, or which foods may be driving delayed immune reactions.
Used properly, a home bloodtype test kit can be useful for personal awareness. Used for the wrong purpose, it can send you in the wrong direction. That’s where many people get stuck.
Why People Use Bloodtype Test Kits
A typical scenario goes like this. Someone has had digestive discomfort for months. They’ve tried cutting dairy, then gluten, then “healthy eating” more broadly. Symptoms improve a little, then return. They start searching online and find claims linking blood group to diet, inflammation, and food tolerance. A bloodtype test kit looks like a sensible first step.
That appeal makes sense. You get an immediate result at home, without booking into a clinic or pathology centre. For some people, it’s also tied to family planning, blood donation interest, or wanting to know basic health information.
What these kits are genuinely good for
A home bloodtype test kit is most useful when the goal is straightforward:
- Personal knowledge: You want to know whether you’re A, B, AB, or O, and whether you’re Rh positive or negative.
- General preparedness: You’d like a rough understanding of your blood group for your own records.
- Education: You want to see how blood typing works in practice.
Blood typing itself has a serious medical history. In Australia, blood type testing became a cornerstone of safer transfusion practice after Karl Landsteiner’s 1901 discovery of the ABO blood group system, and adoption by the Australian Red Cross Blood Service in the 1930s helped reduce transfusion mortality from over 80% pre-1901 to under 1% by the 1940s, according to this historical summary.
Where people get misled
The confusion starts when blood type is treated as a broad health diagnostic.
Practical rule: A blood type result is a classification result, not an explanation for chronic symptoms.
If your real question is, “Why do I feel unwell after eating?” a bloodtype test kit usually won’t help much. It won’t identify delayed food-related immune responses. It won’t map symptom patterns. It won’t replace careful clinical interpretation.
That doesn’t make the kit useless. It just means the tool has a limited job. The more complex your symptoms are, the more important it is to match the test to the question.
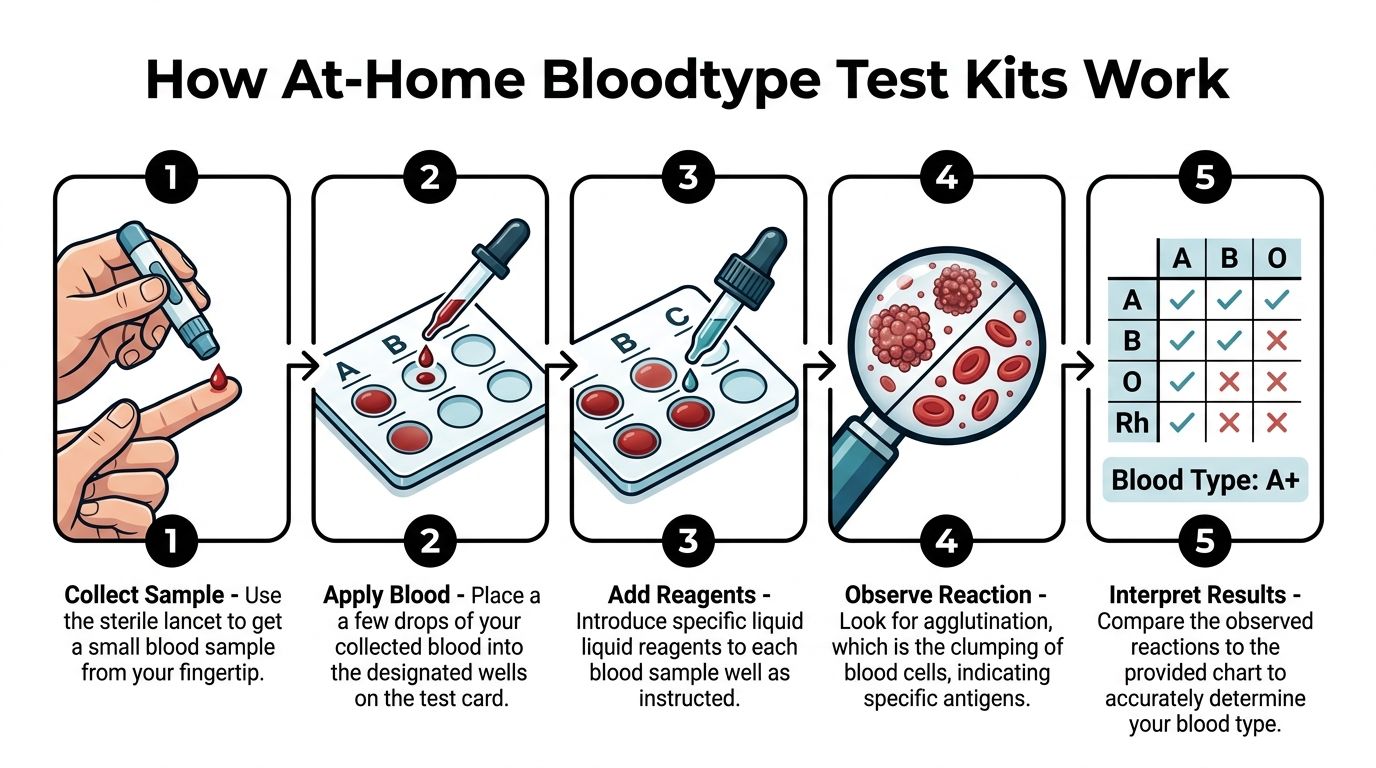
How At-Home Bloodtype Test Kits Work
Most home kits use a method called forward typing. Brands such as EldonCard® use dried antibody sera on a card, including Anti-A, Anti-B, and Anti-Rh, and visible clumping appears within 2 to 5 minutes when the matching antigen is present, as described in the EldonCard product information.
Think of it as a lock-and-key reaction. Your red blood cells carry markers on their surface. The test card contains antibodies designed to recognise those markers. If the right marker meets the right antibody, the cells clump together. That clumping is called agglutination.
What you do at home
The process is simple, but it isn’t forgiving of sloppy technique.
- Clean your finger and prepare the kit. Most kits include a sterile lancet, a test card, and liquid to help the reaction spread properly.
- Prick your finger. You collect a small blood sample.
- Apply blood to the marked test areas. Each area corresponds to a different antibody.
- Add the buffer or water if the instructions require it. This helps the sample mix and react.
- Watch for visible clumping. The pattern of clumping tells you the blood group.
Later in the process, timing matters. So does using enough blood. If too little blood reaches the reaction area, the clumping may be weak and harder to read.
For a technical overview of how clinical blood analysis differs from simple card-based reactions, it helps to review the ImuPro test method.
A short demonstration can make the process easier to visualise:
What the reaction means
Here’s the basic logic:
- Clumping in Anti-A only usually indicates type A
- Clumping in Anti-B only usually indicates type B
- Clumping in both usually indicates type AB
- No clumping in either usually indicates type O
- Clumping in Anti-Rh indicates Rh positive
The Australian context matters too. The same EldonCard product information notes that O+ is the most prevalent blood type in Australia at approximately 37 to 40%, which is useful background but not something that changes how your own kit is read.
If the sample is messy, the timing is off, or one well gets contaminated, the science is still sound but the home result may not be.
That’s the central trade-off. The chemistry is established. The weak point is usually the human using the kit.
At-Home Kits vs Professional Lab Testing
If you're choosing between a home bloodtype test kit and professional testing, the question isn’t which one is “better” in the abstract. The question is what job you need done.
A home kit is built for convenience. Professional testing is built for clinical reliability.
Different tools for different decisions
Home blood typing kits can be useful for quick awareness. But they are not intended for screening prior to transfusion or surgery, and they are not the same as detailed blood analysis performed through professional collection and laboratory handling, as noted by the home blood typing kit guidance here.
That distinction matters more than many people realise. When a practitioner is investigating chronic symptoms, the process matters almost as much as the test itself. Sample handling, stability, lab methodology, and result interpretation all affect whether the result is clinically useful.
| Feature | At-Home Bloodtype Test Kit | Professional Lab Testing (e.g., ImuPro) |
|---|---|---|
| Main purpose | Personal blood group awareness | Clinical investigation |
| Sample collection | Finger-prick done by the user | Professionally collected sample |
| What it measures | ABO and Rh typing | Broader biomarkers depending on the test ordered |
| User error risk | Higher, because the user performs and reads it | Lower, because collection and processing are controlled |
| Suitable before surgery or transfusion | No | Clinical services use formal testing protocols |
| Useful for chronic symptom investigation | Very limited | Yes, when the correct test is selected |
Where home testing falls short
For chronic symptoms, the issue isn’t speed. It’s fit-for-purpose data.
A person with bloating after meals, recurrent migraines, skin flare-ups, or unexplained fatigue doesn’t usually need to know their blood group first. They need to know whether there are delayed food-related immune responses, histamine-related issues, or another pattern worth investigating.
That’s why I often advise clients to be cautious about consumer tests that promise clarity from a very narrow measurement. There’s a useful discussion of this broader issue in low quality food intolerance tests.
A practical way to decide
Use a home bloodtype test kit if your question is simple: “What is my blood type?”
Choose professional testing if your question is clinical: “What’s contributing to my symptoms, and what should I do next?”
Those are not the same question, and they should not get the same test.
Understanding Test Accuracy and Your Results
Manufacturers often present blood type kits as easy and accurate, and many of them are. In real life, though, accuracy depends on both the product and the person using it.
According to the Erycard kit documentation, AU-market blood type kits show 98% accuracy versus lab methods when instructions are followed, but invalid results occur in 2 to 4% of home tests because of user error. The same document notes the use of single-use sterile lancets with 1.8 mm penetration and a 12-month shelf life under suitable conditions.
What tends to affect the result
The common failure points are practical, not mysterious:
- Too little blood: Weak reactions are harder to interpret.
- Poor mixing: The blood and reagent don’t interact properly.
- Reading too early or too late: Timing changes what you see.
- Cross-contamination: Blood from one area spreads into another.
- Ignoring the control well: If the control is invalid, the whole result is unreliable.
How to read the card sensibly
A valid interpretation depends on clear, stable reaction patterns. Persistent clumping in the relevant well indicates that the corresponding antigen is present. No clumping means it is absent.
What matters most is not memorising every pattern. It’s recognising when the result is clean versus ambiguous. If a reaction looks faint, smeared, patchy, or inconsistent with the instructions, don’t force an interpretation.
A doubtful home result should stay doubtful. Confidence is not the same as accuracy.
This same principle applies in broader pathology work. If you want to effectively interpret your lab results, the best approach is always to combine the raw result with context, method, and clinical judgement.
What your result does not tell you
Many people hold misconceptions regarding blood type. Your blood type does not tell you which foods are triggering delayed symptoms. It does not explain IBS-like symptoms, headaches, skin flare-ups, or fatigue. It does not give you a personalised nutrition plan.
For people who are used to seeing complex lab reports, it can also help to understand how practitioners review more clinically relevant findings. This article on IgG food sensitivity test results explained is a useful example of the difference between a simple classification test and a more detailed interpretive process.
Blood Type and Your Health What Science Says
Blood type has become tied to a lot of health claims online, especially around eating patterns. The most popular idea is the blood type diet. It suggests that your ABO group should determine what foods you eat, avoid, or prioritise.
That idea is attractive because it feels personalised. In practice, it’s still a generalised system. It puts people into broad categories and assumes those categories explain symptom patterns. Clinical nutrition rarely works that neatly.
Why blood type is a weak guide for diet decisions
A person’s response to food is shaped by many factors. Symptom timing, immune reactivity, gut health, histamine handling, overall diet pattern, stress, and medical history all matter. Blood type alone doesn’t capture that complexity.
If someone with fatigue and bloating removes foods solely because a blood type chart says they should, two things often happen:
- they remove foods that weren’t causing a problem
- they keep eating foods that do cause problems
That approach can leave people on a highly restrictive diet with no clear symptom improvement.
What personalised nutrition should look like
A useful nutrition plan is based on measurable reactions and symptom context, not broad identity labels. That’s especially true when symptoms are delayed and inconsistent.
The best dietary strategy is not the one that sounds personalised. It’s the one that is actually based on your own biology.
In clinic, that means looking at what the body is doing rather than forcing it into a template. If a person reacts after certain foods, the relevant question isn’t “What does my blood group say I should eat?” It’s “Which foods are associated with my symptoms, and what mechanism is worth investigating?”
A better standard for decision-making
For simple curiosity, blood type information is fine. For chronic symptoms, it’s too blunt an instrument.
That’s why I don’t recommend using a bloodtype test kit to build an elimination diet. A targeted plan should be informed by symptoms, professional review, and where appropriate, clinical testing that can support the classic three-phase process of elimination, provocation, and stabilisation.
Beyond Blood Type Advanced Diagnostic Testing
When someone comes in with longstanding bloating, headaches, skin issues, fatigue, or digestive discomfort, a blood type result doesn’t move the case forward very far. Those symptoms call for testing that can investigate mechanisms linked to the symptom pattern itself.
One important area is Type III delayed food allergy, involving IgG antibodies. This is different from Type I IgE allergy, which is the immediate, potentially anaphylactic pattern commonly associated with the word “allergy.” Delayed reactions can appear well after eating, which makes them much harder to recognise from memory alone.
Why delayed reactions are difficult to identify
A food can be eaten on Monday and symptoms may not become obvious until much later. By then, the connection is blurred. People often blame the wrong meal, the wrong ingredient, or nothing at all.
That’s why broad trial-and-error diets can become frustrating. You remove several foods, feel uncertain, then reintroduce them randomly and end up more confused than when you started.
For this kind of investigation, sample quality and laboratory method matter. The current online discussion around blood type kits often misses Australia-specific guidance about local pathology collection, professional sample handling, and the difference between casual finger-prick testing and protocols designed for delayed food reaction assessment. That lack of clarity is one reason people need better education on why clinical-grade testing matters.
What clinical-grade testing adds
For chronic symptom work, the benefit of a formal process is not just that the test is more advanced. It’s that the whole pathway is more controlled.
A proper work-up may include:
- Professional pathology collection: This improves sample handling and stability.
- Laboratory analysis using ELISA: This is used for assessing specific IgG responses in specialised German laboratories.
- Structured interpretation: Results are used to guide elimination, then provocation, then stabilisation.
- Complementary testing where relevant: DAO enzyme testing may help when histamine intolerance is part of the picture.
What actually helps in practice
The right next step depends on the pattern of symptoms.
If the issue is curiosity about your blood group, a home bloodtype test kit may be enough.
If the issue is recurring symptoms after eating, the more useful path is clinical investigation that can identify potential triggers and support a targeted nutrition strategy. That doesn’t mean chasing every available test. It means choosing one that matches the biological question being asked.
When symptoms are chronic, vague, or delayed, the answer usually comes from better targeting, not more guessing.
Your Next Steps for Taking Control of Your Health
A bloodtype test kit can be worthwhile when you want quick personal insight into your ABO and Rh group. That’s its lane. It’s simple, accessible, and often good enough for curiosity.
But if your real goal is to understand persistent digestive issues, headaches, fatigue, skin flare-ups, or other ongoing symptoms, blood type won’t give you the answers you’re looking for. It’s the wrong tool for that job.
A better approach starts with asking a more precise question. Are you trying to identify a basic blood group, or are you trying to understand food-related symptom patterns? Once that’s clear, the next step becomes much easier.
For chronic symptoms, I’d recommend keeping your focus on personalised, clinically useful data. That may mean discussing delayed food reactions, the distinction between Type III IgG responses and Type I IgE allergy, and whether a structured plan of elimination, provocation, and stabilisation makes sense for you. In some cases, it may also mean looking at complementary markers such as DAO when histamine intolerance is suspected.
You don’t need to guess your way through restrictive diets or rely on blood group theories that oversimplify a complex problem. You need the right test for the right question, plus a practitioner who can interpret the result in context and turn it into a practical plan.
If you’re ready to move beyond a simple bloodtype test kit and investigate chronic food-related symptoms more thoroughly, ImuPro Australia offers clinical-grade IgG food intolerance testing using ELISA analysis in specialised German laboratories, along with complementary options such as DAO testing for histamine intolerance. It’s a practical next step if you want clearer guidance for identifying triggers and building a structured elimination, provocation, and stabilisation plan.