Some people arrive at the question of a histamine intolerance test australia after a long stretch of frustration. Their standard blood work is unremarkable. Allergy testing hasn’t explained much. Yet the pattern keeps repeating. A glass of red wine leads to a pounding head. Leftovers trigger bloating and nausea. A “healthy” avocado toast lunch is followed by flushing, fatigue, or an itchy rash.
That pattern matters, especially when symptoms cross body systems. Histamine intolerance doesn’t usually present as one neat complaint. It can look like migraines, digestive upset, skin flares, sinus symptoms, palpitations, or a vague sense that certain foods just don’t agree with you anymore. Many people start doubting themselves because the reaction isn’t always immediate and it isn’t always dramatic.
The Unseen Trigger for Chronic Symptoms
A common clinical story goes like this. Someone has recurrent headaches, bloating, loose bowels, facial flushing, or skin irritation. They cut out one food, then another, then another. For a week they feel better, then symptoms return for reasons they can’t pin down.
Histamine intolerance is one explanation worth considering when symptoms seem inconsistent but food still looks involved. It isn’t a classic food allergy. It’s better understood as a problem of histamine handling, where the body struggles to break down and clear histamine efficiently.
In Australia, this sits inside a broader and very real food reaction problem. Adverse reactions to food affect approximately 20% of the population, and Australia has some of the highest recorded rates globally, according to Monash University’s review of food allergy and intolerance testing.
When symptoms don’t fit one box
What makes histamine issues so easy to miss is that they can mimic several different problems at once. A person might first see a GP for reflux or bowel symptoms, then a dermatologist for hives or eczema, then blame stress when fatigue and headaches continue.
A few clues often raise suspicion:
- Food patterning such as reactions after aged, fermented, leftover, or alcohol-containing meals
- Multi-system symptoms where gut, skin, head, and energy symptoms overlap
- Negative allergy work-up despite clear food-related symptom flares
- Stop-start improvement with self-directed food restriction that never feels stable
Histamine intolerance often hides in plain sight because the symptoms are real, but they don’t behave like a textbook allergy.
Why people need a clearer path
A lot of advice online is too vague to be useful. Some sources tell people to “just go low histamine” for months. Others push broad wellness testing with little explanation of what is being measured.
That’s not good enough. If food is contributing to symptoms, the process should be grounded in clinical reasoning, not guesswork. Reliable testing in Australia has to answer a practical question. Are we looking at allergy, delayed food reactivity, histamine handling, or something else entirely?
For many patients, the first relief comes from finally having a plausible framework. The second comes from using the right test for the right question.
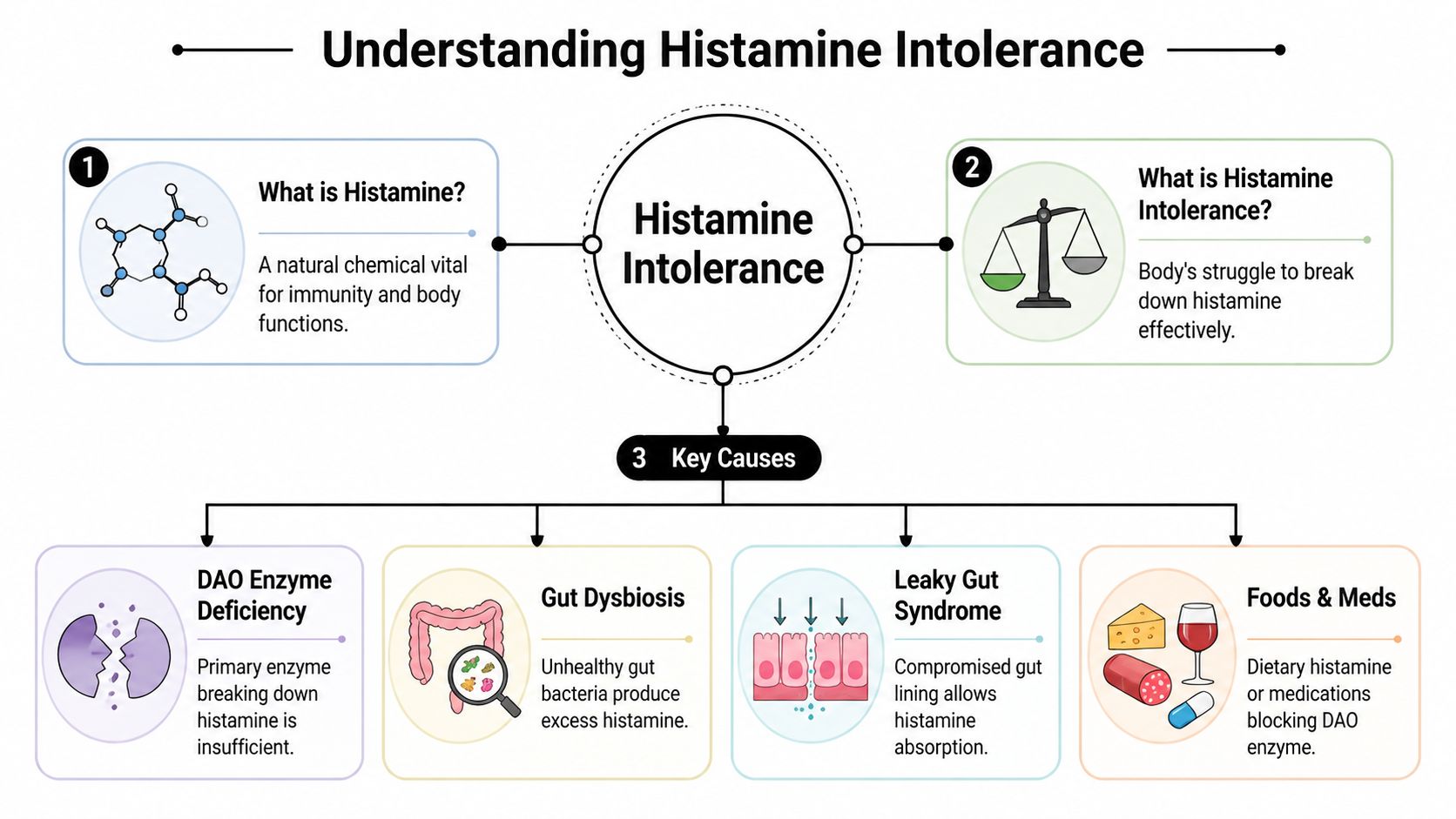
Understanding Histamine Intolerance and Its Causes
Histamine itself isn’t the villain. It’s a normal body chemical involved in immune signalling, digestion, and other everyday functions. The problem starts when the total histamine load rises beyond what your body can comfortably clear.
A useful way to picture it is the histamine bucket. Histamine comes in from food, from your own cells, and sometimes from gut-related triggers. If the bucket fills faster than it drains, symptoms appear.
The main drain is DAO
One of the key “drains” for dietary histamine is diamine oxidase, usually shortened to DAO. This enzyme helps break down histamine in the gut. If DAO activity is low, histamine can accumulate and trigger symptoms that feel allergy-like without being a true IgE allergy.
That’s why DAO testing gets attention. It isn’t measuring whether you’re allergic to a food. It’s looking at a mechanism involved in how your body processes histamine.
For a patient-friendly overview of common symptom patterns, this guide on whether you could be suffering histamine intolerance is a useful starting point.
Why the bucket overflows
DAO deficiency is only part of the picture. Histamine burden can rise for several reasons at once, which is why one person reacts strongly to leftovers and wine, while another mainly struggles with gut symptoms and fatigue.
Common contributors include:
- Reduced DAO activity. Less enzymatic breakdown means dietary histamine is handled poorly.
- Gut dysbiosis. Some gut patterns can increase histamine production or aggravate the gut lining.
- Compromised gut barrier function. A disrupted gut environment can make food reactions harder to interpret and harder to settle.
- Food and medication effects. Some foods are naturally histamine-rich, and some medicines may interfere with histamine handling.
Practical rule: Histamine intolerance is rarely about one “bad” food. It’s usually the combination of total histamine load, enzyme capacity, gut health, and timing.
Why symptoms can seem inconsistent
Patients often say, “But I ate that last week and I was fine.” That doesn’t rule histamine out. If the bucket was relatively empty that day, the same food may have been tolerated. On another day, after stress, poor sleep, alcohol, leftovers, or a string of higher-histamine meals, the threshold may be much lower.
This is also why histamine intolerance shouldn’t be reduced to a single laboratory value. A DAO result can be helpful, but a complete picture comes from combining symptoms, food patterns, and clinical context.
Navigating Testing Options in Australia
A common Australian scenario goes like this. Someone has headaches, flushing, bloating, or a racing heart after wine, leftovers, or aged foods. Their allergy blood tests come back negative, and they are told food is unlikely to be involved. That conclusion is often too broad, because different tests assess different biological pathways.
The first job is to choose the test that matches the question.
What each test measures
| Test Type | What It Measures | Reaction Type | Primary Use |
|---|---|---|---|
| IgE allergy blood testing | Immune response associated with immediate allergy | Allergy | To investigate suspected allergic reactions |
| IgG food testing | IgG antibodies to selected foods | Delayed food reactivity context | To support structured elimination planning in selected cases |
| DAO enzyme activity testing | DAO activity in blood serum | Histamine handling capacity | To assess whether low DAO may be contributing to histamine intolerance symptoms |
IgE tests and why they can be negative
In Australian practice, standard allergy blood tests are appropriate when the concern is a true allergy. ASCIA notes that Medicare rebates are available for IgE-specific allergy tests, but those tests do not diagnose intolerance.
So if symptoms appear after wine, mature cheese, leftovers, or mixed meals and IgE testing is negative, the result points away from IgE-mediated allergy. It does not rule out histamine intolerance, reduced DAO activity, or other non-allergic food reactions.
That distinction matters in clinic. I often see patients who were reassured by a negative allergy panel, yet their symptom pattern still strongly suggests a histamine handling issue.
IgG testing as a complementary tool
IgG food testing answers a different question again. It does not diagnose histamine intolerance, but it can help identify delayed food reactivity patterns in selected patients with chronic, meal-related symptoms.
The trade-off is straightforward. Used with a clear clinical plan, IgG results can support a structured elimination and reintroduction process. Used without context, they can push people into unnecessary restriction and make an already confusing symptom picture harder to interpret.
For a clearer explanation of the difference between these categories, this guide to allergy and intolerance testing outlines how they are used in practice.
Where DAO testing fits
DAO testing is the test category that speaks most directly to histamine intolerance. The key point is methodological. A clinical-grade DAO test measures enzyme activity in serum from a venous blood draw, not a vague wellness marker from an unvalidated consumer screen.
In Australia, ImuPro Australia’s DAO Histamine Intolerance Test is a direct-to-consumer option based on serum analysis of DAO enzyme activity through ISO-certified German laboratory processing and a validated ELISA method, as noted in the company’s technical materials.
That difference is practical, not cosmetic. Venous blood collection through a pathology setting gives a cleaner, more controlled sample pathway than generic at-home wellness testing. If the goal is to assess whether low DAO may be contributing to symptoms, clinical-grade serum testing is the more reliable option.
A search for histamine intolerance test australia should lead to one clear question. Is the test assessing allergy, delayed food reactivity, or DAO function?
What works and what does not
Good testing starts with a symptom pattern, then matches the method to the mechanism being considered.
Problems arise when a single negative allergy test is treated as the end of the investigation, or when broad, poorly validated wellness panels are used in place of pathology-based assessment. Histamine intolerance is already difficult to pin down. The testing process should reduce uncertainty, not add to it.
The Clinical-Grade Testing Process Explained
People are often more comfortable once they understand how the process works. A proper histamine assessment isn’t a casual wellness exercise. It should look and feel like a healthcare pathway.
Australia has a real problem with unproven testing in this space. The Murdoch Children’s Research Institute notes that the country has the world’s highest childhood food allergy rates at 10% among 12-month-olds, and also warns that unproven commercial tests have proliferated despite lacking evidence. Their position is clear that a clinical-grade process involving pathology collection and validated lab analysis is needed, as outlined by MCRI’s work on population allergy.
Step one is clinical context
Before any blood is drawn, symptoms need to be framed properly. That means looking at timing, meal patterns, medication use, alcohol, leftovers, gut symptoms, headaches, skin changes, and whether conventional allergy work-up has already been done.
This first step prevents a common mistake. Patients often assume histamine is the issue because they react to “healthy” foods, but the pattern may also involve FODMAPs, coeliac disease, reflux, biliary issues, or another gut process. Testing is stronger when the clinical question is specific.
Pathology collection and serum analysis
The sample collection should be straightforward and professional:
- A venous blood draw is arranged through a pathology collection setting.
- Blood serum is prepared for analysis, which is the required sample type for DAO assessment discussed in this article.
- The specimen is processed in a validated laboratory, rather than interpreted through an informal wellness workflow.
- Results are returned with context, not just a raw number.
You can see the method details in ImuPro’s test method overview.
Why this process is worth insisting on
There’s a practical reason clinicians prefer pathology collection and laboratory analysis. Pre-analytical handling matters. So does consistency. If you’re trying to evaluate enzyme activity, the method can’t be an afterthought.
A clinical-grade approach gives you:
- Professional collection that reduces sample handling errors
- Serum-based analysis aligned with the intended DAO methodology
- Laboratory validation rather than broad consumer wellness claims
- A cleaner foundation for diet planning and practitioner review
Good testing doesn’t replace clinical judgement. It gives clinical judgement something more reliable to work with.
Interpreting Your Results and Next Steps
A DAO result is useful, but it isn’t a diagnosis by itself. That point is worth holding firmly. Histamine intolerance is still a clinical picture first, and a lab result second.
What low, borderline, or normal results can mean
If DAO activity is low, that may support the suspicion that impaired histamine breakdown is contributing to symptoms. If it’s borderline, the result may still be relevant, especially when the symptom pattern is strong and reactions are reproducible. If it’s normal, histamine intolerance becomes less straightforward, but it isn’t automatically off the table.
That’s because people don’t react to numbers in isolation. They react through the combined effects of diet, gut function, medications, stress, alcohol, sleep disruption, and existing inflammatory burden.
How practitioners put the result to work
The next move is usually not “cut everything out indefinitely.” It’s a structured trial.
A sensible clinical plan often includes:
- A targeted low-histamine elimination phase for a defined period
- Symptom tracking across headaches, bowel symptoms, skin changes, sleep, and energy
- Careful reintroduction to separate true triggers from background noise
- Review of cofactors such as alcohol, leftovers, fermented foods, and medications
The low-histamine dietary trial remains the practical gold standard for confirming whether histamine is relevant. The DAO result helps make that trial more focused and more credible.
Looking for root causes
If someone improves on a lower-histamine plan but keeps relapsing, the next question is usually why the system became reactive in the first place. Broader functional assessment can then be clinically helpful. According to Byron Herbalist’s discussion of histamine intolerance testing and root cause assessment, emerging practitioner consensus in Australia supports integrating DAO results with assessments such as advanced stool testing or Organic Acid Tests when clinically appropriate.
That doesn’t mean every patient needs every test. It means recurring histamine symptoms often deserve a deeper look at gut ecology, infection, mould exposure, or other aggravating factors when the history points that way.
A result only becomes useful when it changes what you do next. For most people, that means a supervised dietary trial and a search for the reason the threshold became so low.
What to avoid after you get results
Two mistakes are common.
The first is treating a result as a label for life. The second is building an excessively restrictive diet around fear. Both can keep people stuck. Histamine-related care works best when it is targeted, time-limited, and reviewed, not when it becomes an endless shrinking list of “safe foods.”
Costs Logistics and Practitioner Collaboration
Cost and logistics often determine whether people follow through with testing at all. In practice, the value of a clinical-grade venous DAO test is not just the number on the report. It is the fact that the sample is collected through a standard pathology process, then interpreted by someone who can relate it to symptoms, diet, medications, and the broader clinical picture.
Turnaround and reporting
Patients usually want to know two things straight away: how the sample is collected, and how long results take. With venous blood draw DAO testing in Australia, collection is typically handled through a pathology pathway rather than an at-home wellness kit. That matters because pre-analytical handling affects specimen quality, and poor handling can make any result less useful.
Turnaround is usually measured in days, not hours.
ImuPro Australia states a laboratory reporting window of 10 to 20 days for its DAO serum testing process. The more important point is what happens after the report arrives. A DAO value on its own has limited meaning unless a practitioner checks whether it fits the history, symptom pattern, and response to food.
What the process looks like in real life
For patients, the logistics are usually manageable:
- Arrange the test through the relevant collection pathway
- Attend a standard venous blood draw
- Allow time for laboratory processing and reporting
- Review the result with a qualified practitioner
- Convert the findings into a clear, time-limited management plan
That final step is where many people either make progress or get stuck.
A good practitioner uses the result to narrow decisions. They can help decide whether a lower-histamine diet is warranted, how strict it needs to be, how long it should run, and whether cofactors such as alcohol, gut symptoms, menstrual timing, medications, or supplements are likely to be affecting tolerance. That is a better use of testing than treating the result as a stand-alone diagnosis.
Working with your practitioner
DAO testing is usually most helpful when symptoms suggest histamine involvement but the explanation is still uncertain. In Australian practice, that often means the person has already tried to identify triggers, has had allergy considered, or has a mixed symptom pattern that does not fit neatly into one category.
The trade-off is straightforward. Ordering a clinical-grade blood test adds cost and a short delay, but it can reduce guesswork and help avoid an unnecessarily restrictive diet. Skipping testing may be reasonable in simple cases. In more persistent or confusing cases, structured testing often gives a cleaner starting point.
For practitioners, DAO testing fits best inside a wider assessment, not outside it. GPs, dietitians, clinical nutritionists, and integrative practitioners can all use the result if they understand its limits and its role. The goal is to make better decisions, not to collect more data for its own sake.
Used properly, practitioner collaboration protects patients from two common problems: under-interpreting a meaningful low DAO result, and overreacting to an isolated number that does not match the clinical history.
Frequently Asked Questions
Do I need to prepare before a DAO blood test?
Preparation should follow the instructions provided with the pathology collection process. If you take regular medication or supplements, don’t stop them on your own. Review them with your practitioner first so the result is interpreted properly.
Is DAO testing covered by Medicare?
The Medicare point that’s clear from Australian allergy guidance relates to IgE-specific allergy tests, which can attract rebates in appropriate settings. That doesn’t mean intolerance testing or DAO testing is automatically covered. Check the current arrangement before booking.
If my DAO result is normal, does that mean histamine isn’t the issue?
Not necessarily. A normal result makes the picture less clear, but it doesn’t override a strong clinical pattern. A practitioner may still consider a structured dietary trial or look for other causes of food-related symptoms.
Should I do DAO testing or just try a low-histamine diet?
Sometimes a careful dietary trial is enough. Testing becomes more useful when symptoms are persistent, the picture is mixed, or you want a more objective starting point before making significant diet changes.
If you’re dealing with recurring headaches, bloating, flushing, skin flares, or fatigue after meals and want a more structured pathway, ImuPro Australia offers blood serum DAO testing through pathology collection, along with related testing options that can be reviewed with your practitioner as part of a broader food intolerance and gut health assessment.