In recent years, the scientific community has been captivated by the relationship between autism spectrum disorder (ASD), the gut microbiome, and delayed food allergies. Autism, a complex neurodevelopmental condition that affects communication, social interaction, and behavior, has long puzzled researchers due to its multifaceted nature. However, emerging evidence suggests that exploring the intricate interplay between the gut microbiome and delayed food allergies could provide valuable insights into the development and management of ASD.
Prevalence of ASD
1 in 52 children under 15 years will be diagnosed with an Autism Spectrum Disorder (ASD), according to the most recent data from the Australian Bureau of Statistics. An enormous growth in autism diagnoses over the last few years has been identified independent of greater autism awareness and diagnosis of milder cases. With this growing problem many concerned parents are turning to dietary measures to reduce their children’s symptoms. In the overwhelming majority of cases, symptoms occur in the form of both gastro-intestinal and mood disturbances.
Children with ASD often suffer with frequent:
- Bloating.
- Excessive production of gas.
- Belching and abdominal pain.
- Diarrhoea.
- Gastric reflux.
- High rates of inflammatory bowel disease.
Addressing these symptoms typically involves treatment with oral antibiotics, which reduce diarrhoea by eradicating clostridium bacteria. However, studies have also shown that within 2 weeks of antibiotic therapy, children’s behaviour deteriorated significantly. There is also the ever growing issue of antibiotic resistance. This therapy is effective as a short term intervention but can potentially worsen gut related symptoms in the long term.
“This improvement is short-lived generating a vicious cycle –
each supplementation of anti-microbial drugs led to disruption
of protective indigenous bacteria¹”
What is the link between autism and the gut microbiome?
The answer lies in what’s now known medically as the gut-brain axis or the gut-microbiome-brain axis. This is the direct connection between intestinal bacteria and enteric neurons – basically a second brain in your gut. We have long understood that our psychological reactions and emotions affect our digestion. However, new evidence is emerging that suggests the inverse is also true – our digestion and gut microbiome directly affects our mood via this axis.
Gut microbiome composition in ASD
Since the gut is such a sensitive factor in ASD pathophysiology, let’s have a look at the bacterial composition in the gut microbiota of ASD children. Compared to their neurotypical counterparts, those with ASD have been shown to have an imbalance of Bifidobacterium, Lactobacillus, Sutterella, Prevotella and Ruminococcs leading to gut dysbiosis. This dysbiosis (a disturbance in quality and quantity of gut microbiota) is seen across a range of other diseases too. For example, gut microbiome dysbiosis is often seen with inflammatory bowel disease like Crohn’s, atopic disease and metabolic conditions.
“Parents of children with ASD often report that behavioural symptoms
tend to overlap with their gut problems.”
What is the connection with delayed food allergies?
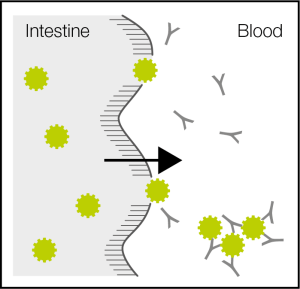
The connection between autism and food allergies is likely to lie in the higher prevalence of intestinal permeability (aka leaky gut) that is seen in ASD patients. A study from 2013 published in BioMed Research International found intestinal permeability was increased in 25.6% of ASDs compared to 2.3% of neurotypical children. This is a significant finding!
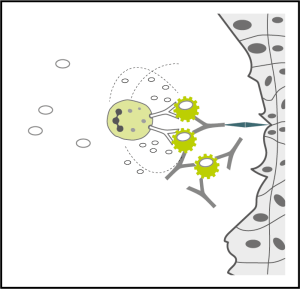
We know that having increased permeability of the intestinal walls allows the passage of larger undigested proteins into the blood. This is responsible for the development of type III allergies or food intolerances. To protect your body from these proteins which have passed through the impaired intestinal barrier, a reaction is launched by the adaptive immune system to form IgG antibodies. Subsequently, the IgG antibodies fix to the food proteins to form an immune complex in the blood stream.
Then, if the immune complex fixes to a tissue it will eventually lead to tissue damage from inflammation. This generated specific symptoms which vary from person to person. This is why it is nearly impossible to identify which food is causing which symptom without testing . If the food forming the immune complex is eaten regularly, a chronic inflammatory reaction is induced in the tissue concerned. This will continue until this food is removed from the diet and the gut lining is restored.
What about gluten and cows milk?
Gluten and casein, the proteins found in wheat (and other grains) and cow’s milk are often high on the list of suspects for many parents. This then prompts them to cut out these foods form their children’s diets in attempt to alleviate ASD related symptoms. However, in our years of experience with IgG testing, it is evident that any food can become a source of inflammation in patients with and without autism. Certainly, it is not always the case that gluten and cow’s milk are the culprits.
As with any allergy, reliable testing is the key to unlock certainty so you don’t need to guess your way to good health.
References:
Szachta P, Bartnicka A, Galecka M & Skonieczna-Zydecka K. 2015. ‘Microbiota disorders and food hypersensitivity in autism spectrum disorders; what do we know?’. in Journal of Experimental and Integrative Medicine. Vol 5
De Magistris, L., Picardi, A., Siniscalco, D., Riccio, M. P., Sapone, A., Cariello, R., Abbadessa, S., Medici, N., Lammers, K. M., Schiraldi, C., Iardino, P., Marotta, R., Tolone, C., Fasano, A., Pascotto, A., Bravaccio, C. 2013. ‘Antibodies against Food Antigens in Patients with Autistic Spectrum Disorders.’ in BioMed Research International. Vol 2013